The Difficulty in Treating Horses
I always say that treating horses brings more benefits to me than to the horses. This makes owners smile, as they only see benefits for the horse. But that is not the truth: there are benefits for me as well. Every day I visit a horse is a new challenge. Every day, horses teach me new things. Every day I must find answers for their musculoskeletal problems, for example, myofascial pain in horses can be challenging for the physiotherapist. The evidence is limited, and we have many questions. Owners ask me:
- “Why is the horse moving like this?”
- ”He is not behaving well.”
- “He is very sensitive”.
- “The vet says imaging tests are fine.”
- “Is he in pain?”
I wonder whether horses have trigger points. Can we find them easily? Are they located near the motor endplate? Do they cause referred pain? Do horses experience referred pain? Which muscles can be needled? Do horses tolerate dry needling? How do they express myofascial pain?
It would be easy if the horse could tell me: “I feel a deep, dull pain that refers down to my groin and sometimes down to my leg that doesn’t go away with painkillers. I’ve been like this for several months.”
Not happening…..
It would be easy if the horse could tell me: “I feel pain in my ear, sometimes it goes up to my eye and when I press near my teeth, it seems to calm down.”
Not happening…..
It would be easy if the horse could tell me: “When I try to move my lower back, I get pain on one side of my spine that feels like it’s going to block my whole back. It scares me to think that I’ll get blocked. And the pain goes all the way up and I feel I cannot breathe.”
Not happening…..
It would also be nice if the owner would tell me: “My horse asked me to call the physiotherapist because he can’t side bend his neck.”
Not happening…..
I may find some answers in the limited scientific evidence regarding equine myofascial pain. If the equine literature leaves me hanging, I may go back to my clinical experience or consult the extensive human trigger point literature. We know, for example, that equine trigger points can be identified, and have similar objective signs and electrophysiological properties as human trigger points (1). We also know that equine trigger points are very common in the axillary portion of the ascending pectoral muscle, and horses may display girth-aversion behavior with more severe trigger points in the area (2).
My horse asked me to call the physiotherapist because he can’t side bend his neck.
Examining Myofascial Pain in Horses
A person will share with a therapist where it hurts, when it hurts, and what the pain is like, but horses can only express themselves nonverbally when something hurts. Clinicians must decode the horses’ expressions. As a prey animal, the horse will try to hide its pain and functional disability whenever it can. It is unlikely that horses under our care will be attacked by a lion or a tiger if they show weakness or pain, but they do not know this for sure. They will always be, act, and feel like prey animals.
Sometimes horses give off subtle signals that something is wrong, and this is common when a horse suffers from myofascial pain. It is not the same if the horse is suffering from colic, ligament injury, or laminitis, for example, and in those cases, the signs of pain are obvious. But if the horse has myofascial pain, the signs will be more subtle. The horse will try to compensate with its body as best as it can. But I have learned to see that they may:
- drag their toes a little
- tilt their head to one side
- shorten their stride a bit
- avoid lateroflexion of the rib cage
- keep the tail hock to one side
- block a scapula
- raise the nape of the neck
- slightly dip the back
The static evaluation, which shares some similarities with the evaluation of people, gives us information about what the horse’s movement is going to be like. We look for asymmetries, postural alterations, muscle imbalances, atrophy, or scars. But it is the dynamic evaluation that will give us more concrete data., just as with people. We observe our patients during sports. We ask for movements that show us their dysfunctions, and we also have specific tests. We watch the horse during walking, trotting, and cantering. We may evaluate the horse on hard and soft ground and vary the left and right hand. If necessary, we may let do the horse do small cavaletti jumps, or going around in small circles, spirals, or and up and down slopes. These observations can help us assess what may be wrong.
Assessing Equine Myofascial Pain with Palpation
Palpation is another powerful tool to examine trigger points. Human intra- and interrater reliability research indicate that the reliability of palpation is high if the clinician has the right skills and experience (3). Maria Resano and I determined that the intrarater reliability of palpation of trigger points in the equine brachiocephalic muscle is acceptable (4). Furthermore, in my clinical experience, nearly 90% of horses express pain on palpation of this muscle, and routinely, I find local twitch responses (LTR) while needling TrPs in horses. Although according to a recent Delphi study (5), LTRs are not a diagnostic criterion, they are very useful as a diagnostic sign, as horses cannot relate to referred pain.
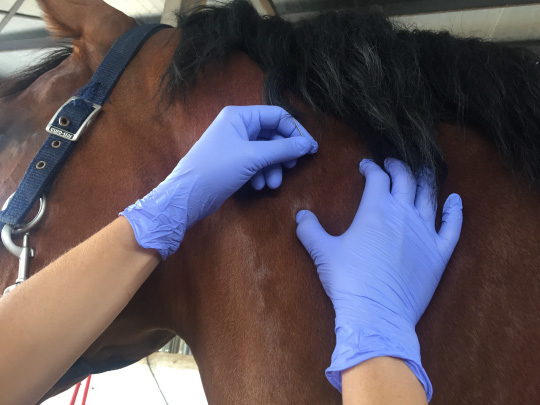
In my equine clinical practice, I rely on palpation to assess myofascial pain in horses. The horses give me feedback with their facial expressions and postures: gestures that I have learned to read through experience and the clues provided by the evidence (5,6,7). The equine muscle is palpated as one would palpate a human muscle. You do not need to be very strong (sometimes people are surprised that a horse physiotherapist is tiny!). I usually use flat and pincer palpation techniques. The horse’s skin, depending on the area, can be very tight and the muscles are large and deep. Therefore, flat palpation is recommended for most muscles and pincer palpation is used more on select muscles such as the brachiocephalic, pectoral, triceps, biceps, and quadriceps muscles.
I use a rather systematic approach when palpating for trigger points, starting at the muscle’s origin and going to the insertion, seeking to gather as much information as possible. Being methodical is important to contrast the different reactions of the horse and the intensity of the responses along the muscle belly, which allows the physiotherapist to locate the most sensitive point. Is it doubtful that taut bands can be palpated in horses, even though palpating a taut band is one of three diagnostic criteria in humans (5)? Just imagine the possible depth of a taut band in the gluteus medius muscle of a horse. Empirically, it is highly questionable and besides, there is no scientific evidence.
Lastly, always listen to the owner.
Treating Trigger Points in Horses with Dry Needling
 Let’s assume that I have already located a hypersensitive spot in the brachiocephalic muscle. As a side note, I choose this muscle for several reasons. It is one of the easiest to palpate with pincer palpation. Usually, it is quite painful and it corresponds kind of to the human trapezius. The muscle is also the subject of my current doctoral studies. I guess you could say, it is my favorite….
Let’s assume that I have already located a hypersensitive spot in the brachiocephalic muscle. As a side note, I choose this muscle for several reasons. It is one of the easiest to palpate with pincer palpation. Usually, it is quite painful and it corresponds kind of to the human trapezius. The muscle is also the subject of my current doctoral studies. I guess you could say, it is my favorite….
If we were to needle a human’s trapezius muscle, the patient would first lie down on the treatment table. Next, we would locate the muscle and the trigger point, ask whether the patient recognizes the pain, and proceed with the dry needling treatment. Horses are usually treated while standing. As we cannot assess whether a horse recognizes provoked pain, we look for all the trigger points and keep needling until the horse feels annoyed or bored. Dry needling requires a lot of patience from the horse.
Horse Reactivity to Dry Needling
Another interesting difference between needling humans and horses is that horses usually are not bothered by the actual needling techniques, which is in stark contrast with most human patients. In humans, dry needling can be rather painful as I know from having needled many of my own muscles! Perhaps surprisingly, horses do not really tolerate the tapping in of the needle, which humans barely notice if at all. Sometimes, I need an assistant to calm the horses by stroking them or giving them a carrot to distract them from the needle insertion. After performing the dry needling techniques, I usually apply percussion massage using a massage gun, which seems to leave the horse with a good feeling. During the next visit, the horse will be happier with the treatment, which is similar to people.
Finally, I recommend that the rider avoids exercises that involve the muscles that have been needling for at least 72 hours following dry needling. Maria Resano and I found that post-needling pain or discomfort decreases after 72 hours (9). When the horse starts his training routine, we would like to be sure that he will not display any dysfunctional movements caused by post-needling pain. I also recommend therapeutic exercise for the treated muscles. The evidence in humans tells us to combine dry needling treatments with therapeutic exercise. At the end of the day, dry needling is very beneficial to our horses.
References
- Macgregor, J., & von Schweinitz, D. G. (2006). Needle electromyographic activity of myofascial trigger points and control sites in equine cleido-brachialis muscle–an observational study. Acupuncture in Medicine, 24(2), 61-70.
- Bowen, A. G., Goff, L. M., & McGowan, C. M. (2017). Investigation of myofascial trigger points in equine pectoral muscles and girth-aversion behavior. Journal of Equine Veterinary Science, 48, 154-160.
- Bron, C., Franssen, J., Wensing, M., & Oostendorp, R. A. (2007). Interrater reliability of palpation of myofascial trigger points in three shoulder muscles. Journal of Manual & Manipulative Therapy, 15(4), 203-215.
- Calatayud-Bonilla, M., Resano-Zuazu, M., & Segura-Ortí, E. (2018). Intra-rater reliability in locating myofascial trigger point in the equine brachiocefalicus muscle. 28 Jornadas de Fisioterapia EUF ONCE; Fascia: Avances Científicos, Madrid.
- Fernández-de-Las-Peñas, C., & Dommerholt, J. (2018). International consensus on diagnostic criteria and clinical considerations of myofascial trigger points: a Delphi study. Pain Medicine, 19(1), 142-150.
- Dyson, S., Berger, J. M., Ellis, A. D., & Mullard, J. (2017). Can the presence of musculoskeletal pain be determined from the facial expressions of ridden horses (FEReq)?. Journal of Veterinary Behavior, 19, 78-89.
- Dyson, S., Berger, J., Ellis, A. D., & Mullard, J. (2018). Development of an ethogram for a pain scoring system in ridden horses and its application to determine the presence of musculoskeletal pain. Journal of Veterinary Behavior, 23, 47-57.
- Gleerup, K. B., Forkman, B., Lindegaard, C., & Andersen, P. H. (2015). An equine pain face. Veterinary anaesthesia and analgesia, 42(1), 103-114.
- Nemery, E., et al. (2016, December). Proceedings of the 9th international symposium on veterinary rehabilitation and physical therapy. In Acta Veterinaria Scandinavica (Vol. 58, No. 2, pp. 95-121). BioMed Central.