Most of us have, at one time or another, experienced voice-related problems. Of course, for singers or teachers symptoms like hoarseness, difficulties producing a strong or normal voice, difficulties reaching that high pitch, or discomfort or pain in the laryngeal region, are particularly challenging. Where do patients go with voice-related issues? Typically, patients will consult first with general practitioners, ear-nose-and-throat (ENT) specialists, laryngologists, or speech therapists, but would a specialized physical therapist, such as a CRAFTA® therapist, be another option?
Voice problems (dysphonia) are prevalent in all ages
The prevalence of voice disorders is variable. Amongst the most reported disorders are laryngitis (8%), vocal fold nodules (VFN), and functional voice disorder (FVD) (both about 20%), and vocal fold paralysis (VFP) (14%). While nodules are mostly seen in young people, VFP and FVD are more commonly observed in the elderly. In adults, FVD is the most prevalent disorder (De Bodt et al. 2015).
Different types of dysphonia are described, but an international unified classification system for dysphonia is still lacking
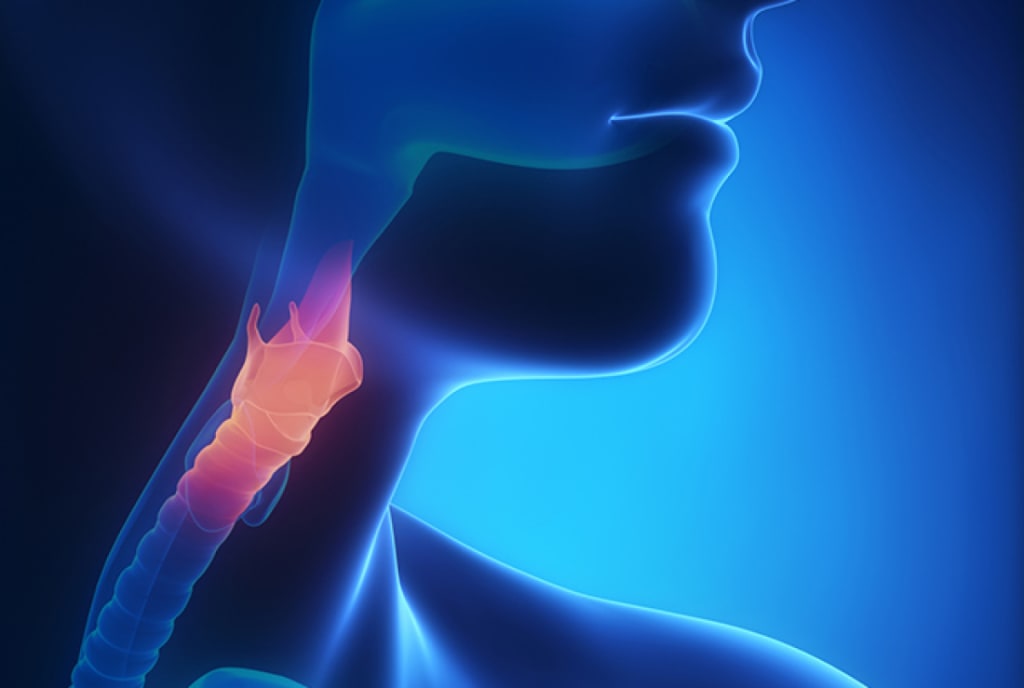 There are some generally accepted classification systems for Functional Dysphonia (Morrison, Rammage, 1993), and they describe typical features seen during inspection of the vocal folds. Researchers criticize these classifications because clinical features seen in functional dysphonia are also seen in people without functional dysphonia (Sama et al. 2001). Typical for functional voice disorders are high tonus of the muscles that surround the larynx, altered activity pattern of infra- and suprahyoid muscles, and postural changes. All these connections, including the laryngeal muscles, play an important role in the functionality of the vocal folds. Alteration of normal functional patterns can have detrimental effects on voice production.
There are some generally accepted classification systems for Functional Dysphonia (Morrison, Rammage, 1993), and they describe typical features seen during inspection of the vocal folds. Researchers criticize these classifications because clinical features seen in functional dysphonia are also seen in people without functional dysphonia (Sama et al. 2001). Typical for functional voice disorders are high tonus of the muscles that surround the larynx, altered activity pattern of infra- and suprahyoid muscles, and postural changes. All these connections, including the laryngeal muscles, play an important role in the functionality of the vocal folds. Alteration of normal functional patterns can have detrimental effects on voice production.
Voice disorders are categorized in structural and non-structural voice disorders
Some examples of structural voice disorders are laryngitis, VFN, polyps, VFP, trauma, or tumors. Functional Voice Disorders (FVD), such as psychogenic or puberphonia disorder, are examples of non-structural voice disorders. Vocal nodules may be a result of a functional voice disorder, but it is still not elucidated whether organic lesions lead to FVD or whether FVD leads to organic pathology (Van Houtte et al. 2011).
What are the main symptoms of functional dysphonia?
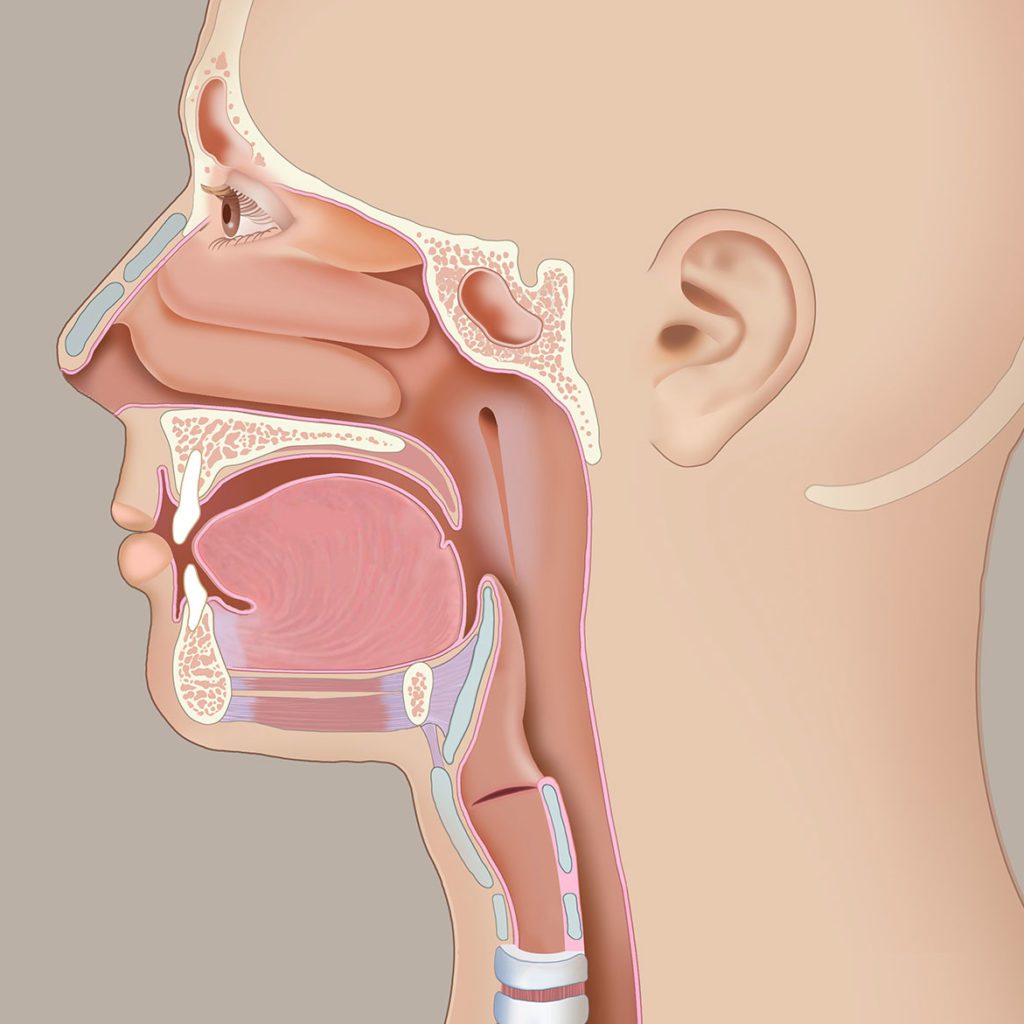 Dysphonic patients often described hoarseness as the cardinal symptom. Clinical features may include changes of the voice, such as fatigue, a weakened or a low voice, problems with pitch levels, volume, range, and nasality. Furthermore, patients may experience pain in the laryngeal region or radiating to the ear, coughing, problems with respiration, swallowing difficulties, and globus sensations (a feeling of “having a lump” in the throat). Research shows that dysphonia has a negative impact on the quality of life (Bassi et al. 2011). Voice related professions like teachers and professional singers are at increased risk.
Dysphonic patients often described hoarseness as the cardinal symptom. Clinical features may include changes of the voice, such as fatigue, a weakened or a low voice, problems with pitch levels, volume, range, and nasality. Furthermore, patients may experience pain in the laryngeal region or radiating to the ear, coughing, problems with respiration, swallowing difficulties, and globus sensations (a feeling of “having a lump” in the throat). Research shows that dysphonia has a negative impact on the quality of life (Bassi et al. 2011). Voice related professions like teachers and professional singers are at increased risk.
Considering the functional chain
In daily practice, neuro-musculoskeletal therapists see many patients with posture-related problems, neck problems, headaches, and cranial or temporomandibular related problems. Often they complain of voice problems as well, maybe not as the primary symptom or perhaps as a delayed clinical feature. Such complaints commonly go by unnoticed because patients may not always mention these symptoms during the initial examination. They may not realize that these symptoms or complaints in other regions of the body may be related to their main problem. Therapists may do not ask more specific questions, possibly because of a lack of knowledge in this field.
Speech-language pathologists and voice therapists do see patients with voice problems who also have widespread postural and functional muscular alterations. There is no reliable research on how these factors may be correlated. Nevertheless, altered muscle activity, altered posture, and loss of mobility and flexibility are clinical features that often can be observed in these patient groups.

In the case of FVD, voice therapy offered by voice therapists mainly consists of indirect voice therapy, i.e., education, vocal hygiene, and direct voice therapy with the main focus on posture, breathing, phonation, articulation, and muscle tension that combined may have better results than no treatment (Van Houtte et al., 2011, Ruotsalainen et al., 2007, 2008).
Voice research traditionally focuses on the vocal tract, articulators, and the larynx, thereby missing a broader scope of the direct and indirect biomechanical and functional relationship of the skull, cervical spine, and sternum.
Several authors have described the extensive correlations between the airway, the craniofacial structures, the cervical spine, and vocal structures. They emphasize the need to consider the function of the vocal structures and the airway in the broader context. Craniocervical postural changes and mandibular positions do influence the function of swallowing and phonation (Sakuma 2010, Furuya et al. 2011, Nakayama et al. 2013). Some aspects of postural alignment differ between normal and dysphonic speakers.
Specialized (Craniofacial) CRAFTA® therapy of the laryngeal region
 Before the treatment by a physical therapist, serious pathologies must be ruled out by either an ENT specialist or a speech pathologist. Next, dysfunctions of the structures responsible for a normal voice may likely play a significant role. In this case, the treatment by a skilled CRAFTA® therapist, in collaboration with a speech or voice pathologist or therapist, may be useful. To become a CRAFTA® therapist may take 3-4 years. The CRAFTA education, in the US hosted by Eureka Seminars, educates students to become specialized craniofacial therapists, who will be able to examine and manage patients with voice problems. The actual therapy consists of manual therapy, specific exercises, and coaching of the voice, often in collaboration with other disciplines.
Before the treatment by a physical therapist, serious pathologies must be ruled out by either an ENT specialist or a speech pathologist. Next, dysfunctions of the structures responsible for a normal voice may likely play a significant role. In this case, the treatment by a skilled CRAFTA® therapist, in collaboration with a speech or voice pathologist or therapist, may be useful. To become a CRAFTA® therapist may take 3-4 years. The CRAFTA education, in the US hosted by Eureka Seminars, educates students to become specialized craniofacial therapists, who will be able to examine and manage patients with voice problems. The actual therapy consists of manual therapy, specific exercises, and coaching of the voice, often in collaboration with other disciplines.
Subjective examination
The subjective examination consists of taking a thorough and detailed history, which often provides essential clues to understand the nature of the patient’s problem better. The interview should not just focus on identifying the source of the symptoms but also aim to understand the underlying pathobiological processes, contributing factors, and possible contraindications. The therapist must gather enough information to develop an informed point of view regarding the prognosis.
Physical examination
 In the absence of a clear etiology, one has to judge the dysfunctions found on examination on their relevance to the patient’s complaints. Sound clinical reasoning, which is the clinical decision process done by the therapist, provides the well-educated and trained CRAFTA® therapist with the ability to make clinical judgments to reach an optimal examination and treatment plan. Different from speech pathologists and voice therapists, CRAFTA® therapists are trained in and capable of screening a broader context, the craniocervical-, craniofacial-, temporomandibular-, shoulder girdle-, thoracic regions, and the neural attachments of the cranial nervous system.
In the absence of a clear etiology, one has to judge the dysfunctions found on examination on their relevance to the patient’s complaints. Sound clinical reasoning, which is the clinical decision process done by the therapist, provides the well-educated and trained CRAFTA® therapist with the ability to make clinical judgments to reach an optimal examination and treatment plan. Different from speech pathologists and voice therapists, CRAFTA® therapists are trained in and capable of screening a broader context, the craniocervical-, craniofacial-, temporomandibular-, shoulder girdle-, thoracic regions, and the neural attachments of the cranial nervous system.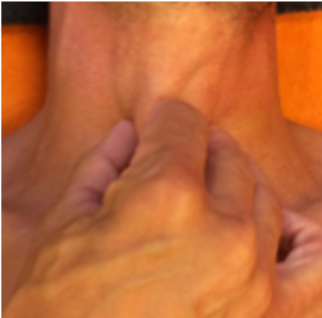
Specific techniques and differentiation tests are used to examine the relationship between the voice problem and dysfunctions found in these connected regions. One aspect of specialized examination and treatment lies in the specific mobilization of the laryngeal structures such as the laryngeal muscles and joints. Unique are the specific mobilization- and palpation techniques for the cranial nerves that innervate this region.
The clear goal of therapy
… should be to minimize the related dysfunctions and contributing factors that play a role in voice problems. Therapy should, therefore, contain not only passive hands-on techniques but also hands-off parts, e.g., specific exercises, stress-reduction, and above all, good explanations to the patient to reach an optimal treatment outcome. Therapy is not about prescribed recipes but must consist of a tailor-made individual examination and treatment plan, which include a multi-structural approach and collaboration with other healthcare disciplines.
Is there evidence for manual therapy around the voice box (laryngeal region)?
Research on the effect and treatment outcomes is growing. A few fairly recent studies show positive effects of manual treatment of the laryngeal region, manual therapy, and exercise in case of dysphonia (Van Lierde et al. 2004, Speyer 2008, Ruotsalainen et al. 2009, Mathieson et al. 2009, Tomlinson 2015, Craig et al. 2015).
Clinical examples of possible causes that can play a role in the development of dysphonia and that easily could be missed are seemingly minor nerve pathologies, such as minor neuropathies after whiplash trauma, excessive traumatic neck extension, or prolonged antero-position of the head. They could comprise the function of the cranial nerves and other structures that are responsible for a normal voice and may contribute to the development of functional voice problems.
Once a colleague told me, “When your instrument, your guitar doesn’t sound that well, you can exercise to play it better or go to a specialist, a mechanic who fixes or tunes your instrument. But what if your voice isn’t working properly?”
When a patient does not seem to benefit from specialized therapy, a more comprehensive screening of the patient’s voice instrument may be indicated, such as the laryngeal region, and its functional connections.
Roald Luning, PT, OMT, Int. CRAFTA® teacher, and Harry von Piekartz, PT, PhD
References
De Bodt M, Van den Steen L, Mertens F, et al. Characteristics of a Dysphonic Population Referred for Voice Assessment and/or Voice Therapy. Folia Phoniatr Logop. 2015;67(4):178–186. doi:10.1159/000369339
Morrison MD, Rammage LA. Muscle misuse voice disorders: description and classification. Acta Otolaryngol. 1993;113(3):428–434. doi:10.3109/00016489309135839
Sama A, Carding PN, Price S, Kelly P, Wilson JA. The clinical features of functional dysphonia. Laryngoscope. 2001;111(3):458–463. doi:10.1097/00005537-200103000-00015
Van Houtte E, Van Lierde K, Claeys S. Pathophysiology and treatment of muscle tension dysphonia: a review of the current knowledge. J Voice. 2011;25(2):202–207. doi:10.1016/j.jvoice.2009.10.009
Bassi IB, Assunção AÁ, de Medeiros AM, de Menezes LN, Teixeira LC, Côrtes Gama AC. Quality of life, self-perceived dysphonia, and diagnosed dysphonia through clinical tests in teachers. J Voice. 2011;25(2):192–201. doi:10.1016/j.jvoice.2009.10.013
Ruotsalainen JH, Sellman J, Lehto L, Jauhiainen M, Verbeek JH. Interventions for treating functional dysphonia in adults. Cochrane Database Syst Rev. 2007;(3):CD006373. Published 2007 Jul 18. doi:10.1002/14651858.CD006373.pub2
Ruotsalainen J, Sellman J, Lehto L, Verbeek J. Systematic review of the treatment of functional dysphonia and prevention of voice disorders. Otolaryngol Head Neck Surg. 2008;138(5):557–565. doi:10.1016/j.otohns.2008.01.014
Sakuma T, Kida I. Relationship between ease of swallowing and deglutition-related muscle activity in various postures. J Oral Rehabil. 2010;37(8):583–589. doi:10.1111/j.1365-2842.2010.02084.x
Furuya J, Tamada Y, Suzuki T. Effect of mandibular position on three-dimensional shape of the oropharynx in seated posture. J Oral Rehabil. 2012;39(4):277–284. doi:10.1111/j.1365-2842.2011.02263.x
Nakayama E, Tohara H, Hiraba H, et al. Effects of reclining posture on velopharyngeal closing pressure during swallowing and phonation. J Oral Rehabil. 2013;40(6):450–456. doi:10.1111/joor.12050
Van Lierde KM, De Ley S, Clement G, De Bodt M, Van Cauwenberge P. Outcome of laryngeal manual therapy in four Dutch adults with persistent moderate-to-severe vocal hyperfunction: a pilot study. J Voice. 2004;18(4):467–474. doi:10.1016/j.jvoice.2004.02.003
Speyer R. Effects of voice therapy: a systematic review. J Voice. 2008;22(5):565–580. doi:10.1016/j.jvoice.2006.10.005
Mathieson L, Hirani SP, Epstein R, Baken RJ, Wood G, Rubin JS. Laryngeal manual therapy: a preliminary study to examine its treatment effects in the management of muscle tension dysphonia. J Voice. 2009;23(3):353–366. doi:10.1016/j.jvoice.2007.10.002
Tomlinson CA, Archer KR. Manual therapy and exercise to improve outcomes in patients with muscle tension dysphonia: a case series. Phys Ther. 2015;95(1):117–128. doi:10.2522/ptj.20130547
Craig J, Tomlinson C, Stevens K, et al. Combining voice therapy and physical therapy: A novel approach to treating muscle tension dysphonia. J Commun Disord. 2015;58:169–178. doi:10.1016/j.jcomdis.2015.05.001