Medial Knee Pain With Running
For a seemingly simple joint, one that allows two degrees of motion, the knee can sometimes be complicated in its presentation. Each year, nearly 10 million women visit their physicians for knee pain. Often the problem is within the knee and other times it is not. Within the last year, I have seen similar patterns within three different female runners of varying ages. They are the subject of this blog.
Three individual cases, one of a 17-year-old competitive high school runner, a second of a 35-year-old running mother and former marathoner, and a third of a 42-year-old female officer in the United States Army, reported right medial and medial-inferior knee pain with running. The women were right-handed.
Symptoms: Medial and Inferior-Medial Knee Pain
The patients reported medial and inferior-medial knee pain with running and they had stopped training because of pain. They were seen for PT previously for “hip weakness” and treated using hip stabilization exercises, including a combination of clamshell exercises and single leg stance exercises targeting the “weak” leg. The single-leg stance exercises were performed placing the involved foot/leg in the middle of a star or clock while the other leg reaches for a corner of the star or a particular number. None of them were able to perform the exercise successfully or without great difficulty and pain.
Examining the Runners
The patients presented with full, pain-free knee flexion/extension. The ligaments were found to be intact and painless with stress testing. All women presented with SI hypomobility in the left SI joint and hypermobility in the right. They presented with trigger points in the right gluteus medius and minimus, and the right QL, right VMO, and lateral quads. All presented with normal patellar mobility. None had any irregularities with imaging.
Treatment
Before treatment, each woman performed a functional pre-test of a 90-degree squat, and a single leg stance for pain, coordination, and stability with and without slight knee flexion (just breaking locking of the knee and back)
Treatment One: Dry Needling to the Gluteus Medius and Minimus
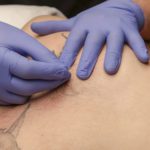
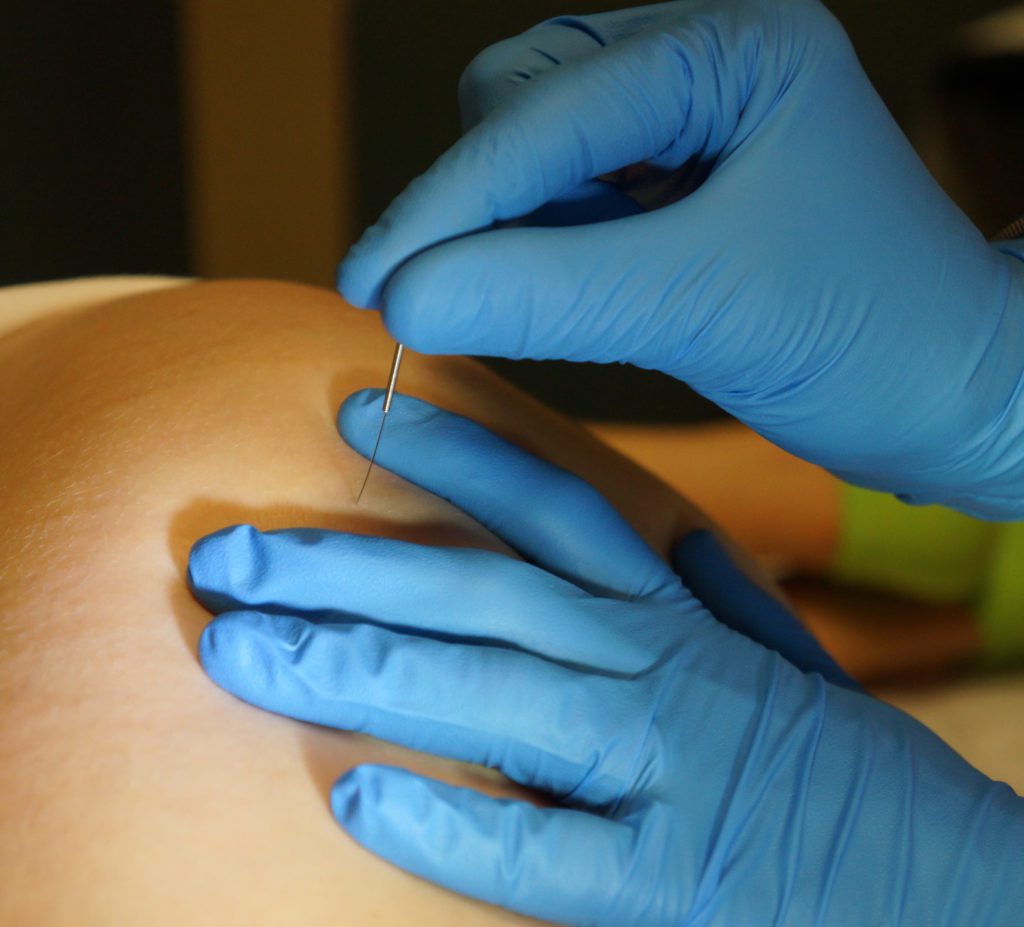 The initial treatment started with each patient in prone. I performed soft tissue manipulation to the QL, bilaterally, followed by a stretch and a gapping technique applied to the left SI joint. Next, I performed deep dry needling (DDN), per Myopain Seminars instructions, to the gluteus medius and minimus, followed up with a posterior hip stretch. The women perform post-tests of squatting and single leg-stance.
The initial treatment started with each patient in prone. I performed soft tissue manipulation to the QL, bilaterally, followed by a stretch and a gapping technique applied to the left SI joint. Next, I performed deep dry needling (DDN), per Myopain Seminars instructions, to the gluteus medius and minimus, followed up with a posterior hip stretch. The women perform post-tests of squatting and single leg-stance.
The 17-year-old and 35-year-old stated they felt more stable and had less pain but still had medial knee pain. They were treated more with DDN to the VMO, triggering multiple local twitch responses, which resolved the remaining knee pain. The 42-year-old stated she had pain in the gastrocnemius, which was also treated with DDN, again triggering multiple twitch responses.
HEP: All women were instructed to abandon their star or clock single-leg exercise. Instead, they were instructed to perform bilateral squats as to not stress their SI joints but to facilitate all the muscles that were treated in the LB and LE.
Treatment Two: Trigger Point Treatment in Vastus Medialis Using Dry Needling
The women returned two days later with significantly less pain. A re-assessment included looking for trigger points in the QL, hip musculature, and quads, and checking the mobility of the SI joint.
The 17-year-old reported being pain-free and anxious to get back to running. Trigger points were treated in her VMO using DDN, and she was instructed to continue with her squats and assigned single-leg, supported (holding onto the counter) shallow, pain-free squats. The 35-year-old also reported a significant reduction in pain but attempted lunges (on her own), which caused her knee pain to return. Her SI joint and involved musculature were treated just as in the first treatment. She then performed bilateral squats, also as a HEP. The 42-year-old reported being able to walk, negotiate stairs and walk pain-free until the day of treatment. She was also treated as in the first treatment.
Treatment Three: Dry Needling to the Gastrocnemius Muscle
Two days after the second treatment, the 17-year-old was pain-free, and she had run 3 miles without pain. Her initial findings were non-problematic. She was instructed to continue her single leg stance exercises for proprioception training but was released to run at will. The 35-year-old had not run or performed lunges but reported no knee pain. She was re-assessed, and her lateral quads were treated with DDN with multiple twitch responses. She performed bilateral squats without any pain, shallow, single-leg squats without pain, and was able to demonstrate a shallow lunge without pain. All exercises were added to her HEP.
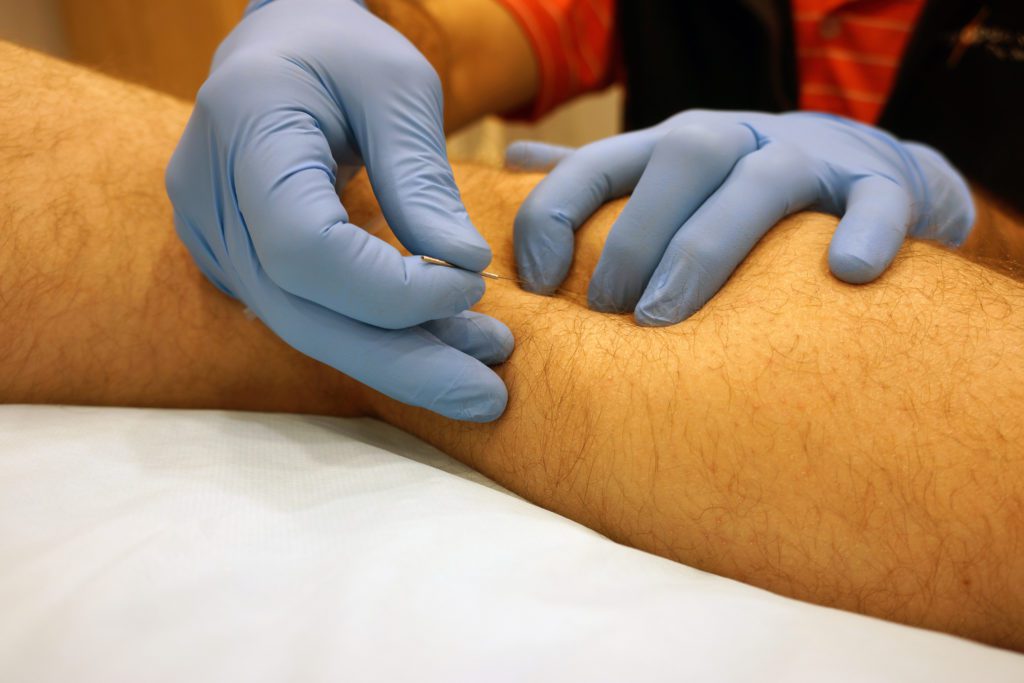 The 42-year-old reported no knee pain but instead mentioned gastrocnemius tightness/pain. She was re-assessed, her left SI was thought to still be slightly hypermobile and was treated. Her gastrocnemius was treated using DDN with multiple twitch responses.
The 42-year-old reported no knee pain but instead mentioned gastrocnemius tightness/pain. She was re-assessed, her left SI was thought to still be slightly hypermobile and was treated. Her gastrocnemius was treated using DDN with multiple twitch responses.
After a standing self-stretch to the gastroc, she was asked to perform bilateral squats, a single-leg stance without any flexion, and a shallow lunge. She was able to do all activities without pain. She completed her visit by running on the treadmill for 5 minutes without pain (time did not permit more). Her goal was to be able to complete her two-mile PE test run and she was released to try a short run or run/walk.
Treatment Four: Myofascial Manipulation to the Hip Musculature, Quads, and Short Hip Adductors
The 35-year-old returned 4 days after the third treatment and reported fatigue in her hip but no pain. She was re-assessed and treated with myofascial manipulation to the hip musculature, the quads, and short hip adductors. Following, she was able to perform bilateral squats, single-leg shallow squats, and lunges without pain. She was able to demonstrate step-downs and plyometrics, skipping in the clinic pain-free, and was released to attempt a short run. The 42-year-old returned 3 days post-treatment three reporting being able to run 1.5 miles at a 14 min pace without pain. She was pleased she could run but disappointed in her cardio condition and was released to slowly train.
Treatment Five: Ongoing Treatment Toward Back
The 35-year-old returned two days after the fourth treatment reporting she was able to run a 12-minute mile with her son. She reported no pain in the lower extremity but irritated her back. She was re-assessed and all previous issues around the pelvis and LE appeared to be resolved. Her treatment was then directed toward her back and she is still receiving treatment at the time of the writing of this blog.
Patterns Identified in the Runners
The purpose of this blog was to share similar patterns seen in female runners of varying ages. The patterns seemed interesting based on the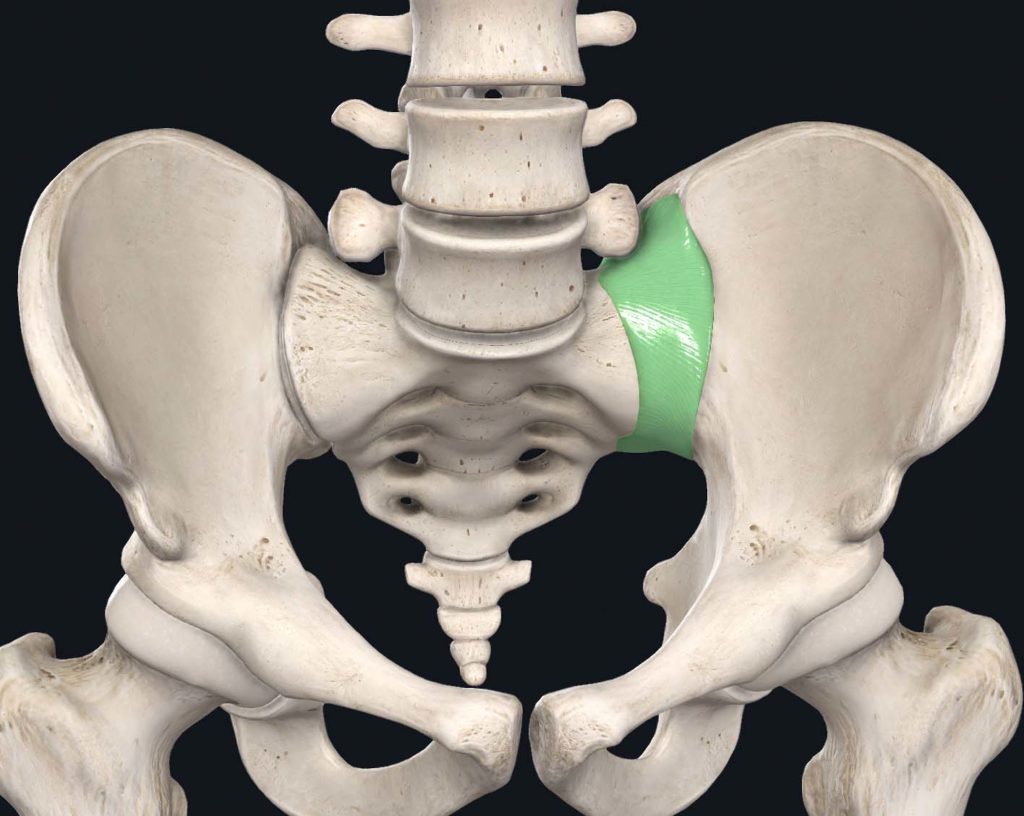 biomechanical principle of force/form closure of the pelvis by Andry Vleeming. My conclusions and clinical reasoning were that the form closure of the SI joint ligaments failed for an unknown reason making it more dependent on force closure, which overloaded the surrounding musculature, i.e., QL and hip musculature. It was interesting to me that none of the women yet presented with psoas issues, which I’ve also seen in such cases.
biomechanical principle of force/form closure of the pelvis by Andry Vleeming. My conclusions and clinical reasoning were that the form closure of the SI joint ligaments failed for an unknown reason making it more dependent on force closure, which overloaded the surrounding musculature, i.e., QL and hip musculature. It was interesting to me that none of the women yet presented with psoas issues, which I’ve also seen in such cases.
Because of the hypermobility in the right SI joint, the quads seemed to have kicked in and been overloaded, most likely trying to stabilize the knee due to the inhibition of the gluteal musculature, lack of hip control, and increased genu valgus with running. Although the star and clock exercises seemed appropriate, they were unsuccessful without first treating the myofascial trigger points, which no doubt, inhibited the hip musculature, and effecting the hip stability. Once the trigger points were resolved and the SI joint balance restored, stabilization training could be utilized and have more chance of success.
Rob Stanborough, PT, DPT, MHSc, MTC, CMTPT, FAAOMPT
Cover photo by Fitsum Admasu on Unsplash