Dry Needling by Athletic Trainers
Dry needling is commonly used by a wide variety of practitioners, including physical therapists [1], occupational therapists [2], acupuncturists [3], chiropractors [4], physicians, dentists [5], veterinarians [6], and more recently athletic trainers [7], among others. In this blog, we will discuss the use of dry needling by athletic trainers.
Although it may make sense for athletic trainers to be able to use dry needling, several athletic trainers’ state boards have either not yet approved dry needling by athletic trainers, such as Tennessee (June 13, 2022), or do not have a defined position on the topic. Several states have already approved dry needling by athletic trainers or are about to approve this. Athletic trainers in California may be able to use dry needling already, primarily because athletic trainers are not regulated by any state board in California. It is, however, conceivable that the California Board of Acupuncture would consider dry needling to be illegal for anyone other than physicians and acupuncturists. Maryland approved dry needling by athletic trainers as of October 2023. authorizing the State Board of Physicians to register licensed athletic trainers to perform dry needling upon completing the appropriate training and education. In Arizona, AZ SB 1398, which has already passed, allows athletic trainers to perform dry needling with the appropriate education and training. North Carolina released a statement on dry needling that allows athletic trainers to perform dry needling with 54 hours of BOC-approved dry-needling training, similar to Nevada regulations, which became effective in late 2020. Myopain Seminars is an approved BOC continuing education provider (Approval Number P8248) .
In Nevada, the qualifications include completing at least 150 hours of didactic education and training in dry needling and submitting documentation with proof of completion to the Nevada State Board of Athletic Trainers. The education requirement includes at least 25 hours of didactic education and training in dry needling provided through an approved postgraduate course of study that requires the successful completion of in-person written and practical examinations. In addition, at least 125 hours can be in approved graduate-level courses or postgraduate continuing education courses in appropriate areas of study relevant to dry needling. Before performing dry needling, an athletic trainer must submit to the Board documented proof of compliance with the qualifications listed in R053-19 using the Dry Needling Verification Form.
In 2015, the AT Strategic Alliance determined that the minimum professional degree level will be a master’s, but the transition from a bachelor’s degree has not yet been completed [8]. Nevertheless, over 70 percent of athletic trainers hold at least a master’s degree. Whether a bachelor’s degree in athletic training is sufficient to cover the minimum amount of education in anatomy, physiology, pain science education, bloodborne pathogen protocols, neurophysiology, etc., is not clear. The Analysis of Competencies for Dry Needling by Physical Therapists identified 123 dry needling competencies [1].
Hortz et al. (2019) published an expert-opinion comparison of the competencies outlined in the “Analysis of Competencies for Dry Needling by Physical Therapists” [1] and the “2020 Standards for Accreditation of Professional Athletic Training Programs” [9], and the “Athletic Training Education Competencies – 5th Edition” [10]. They concluded that “89% of the dry needling tasks were “provided through entry-level education” within the AT 5th Edition Competencies/will be taught through the CAATE 2020 Standards and 11% were not “provided through entry-level education” by AT 5th Edition Competencies/CAATE 2020 Standards and were therefore deemed ‘dry needling specific’.” According to Caramagno et al. (2015), 86% of the 123 competencies are included in the education of physical therapists. The instructors at Myopain Seminars commend the direction and efforts taken in establishing Athletic Training educational standards and competencies; however, unlike the physical therapy analysis, the athletic training review of dry needling competencies was not established by an independent agency. One of the authors of the paper is a dry needling course provider.
The National Athletic Trainers Association (NATA) has issued a Dry Needling Fact sheet, confirming that “there is no profession-wide standard that defines athletic trainer  competence in dry needling” [11]. As was the case in physical therapy, we anticipate that eventually, a growing number of athletic training state boards will approve dry needling, but in the meantime, “athletic trainers must ensure their state practice act does not prohibit them from performing dry needling as part of the athletic training plan of care” [11]. As a side note, the NATA Dry Needling Fact sheet is not entirely up-to-date and appears to have been issued around a decade ago. More recently, the Board of Certification (BOC) for Athletic Trainers has approved Myopain Seminars as an approved continuing education provider (Approval Number P8248) and has awarded continuing education units for Myopain Seminars dry needling courses.
competence in dry needling” [11]. As was the case in physical therapy, we anticipate that eventually, a growing number of athletic training state boards will approve dry needling, but in the meantime, “athletic trainers must ensure their state practice act does not prohibit them from performing dry needling as part of the athletic training plan of care” [11]. As a side note, the NATA Dry Needling Fact sheet is not entirely up-to-date and appears to have been issued around a decade ago. More recently, the Board of Certification (BOC) for Athletic Trainers has approved Myopain Seminars as an approved continuing education provider (Approval Number P8248) and has awarded continuing education units for Myopain Seminars dry needling courses.
Myopain Seminars is an approved BOC continuing education provider.
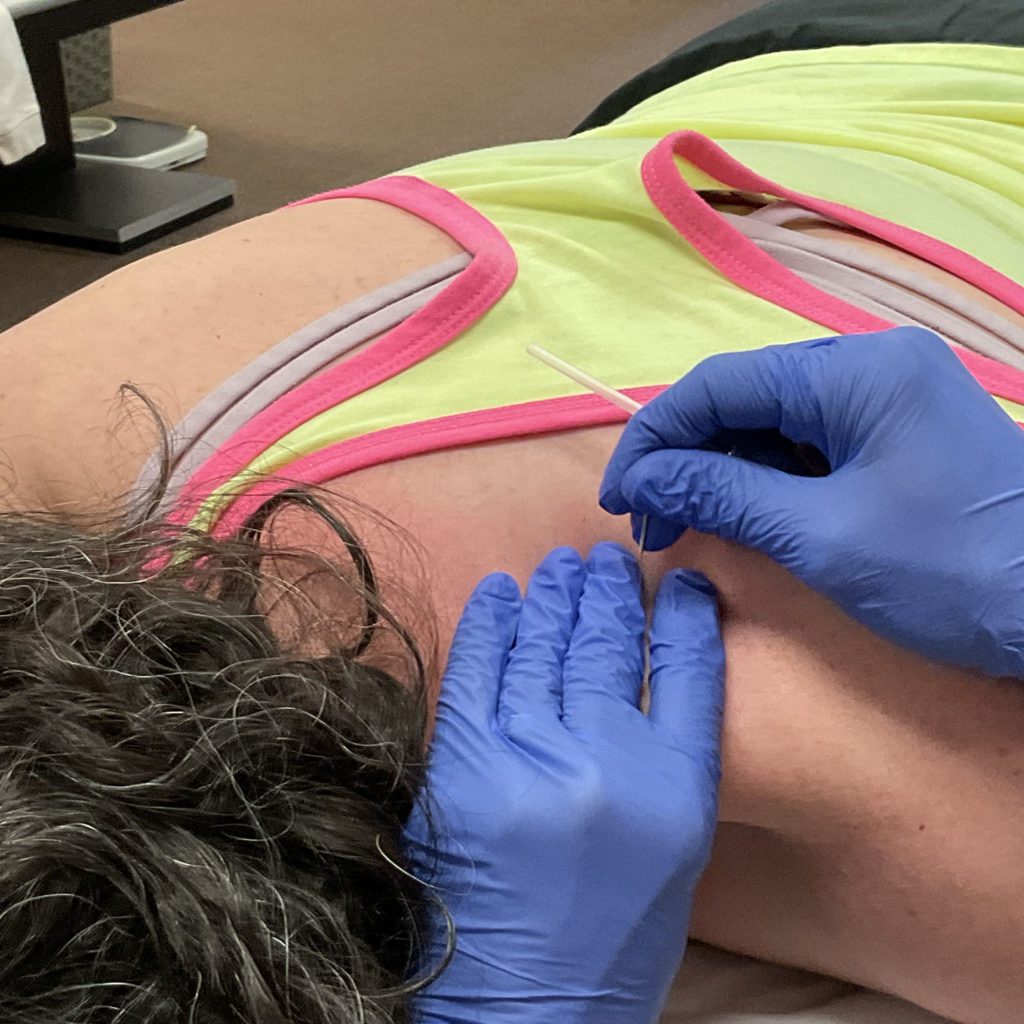 Athletic Training: Prevention, Maintenance, and Performance Enhancement
Athletic Training: Prevention, Maintenance, and Performance Enhancement
Although athletic trainers are relatively new in offering dry needling to their clients, there is increasing evidence that athletes can benefit significantly from dry needling. Athletic training consists of treatment and care for injury prevention, maintenance, and enhancement of athletic performance. Dry needling is an effective treatment in all aspects of athlete care [12]; however, historically, athletic trainers have been restricted to superficial, nonspecific manual techniques with diminished results compared to dry needling [13].
Many clinicians, including athletic trainers, may not realize that injuries are often the result of muscle overload, including sustained or repetitive low-level muscle contraction, eccentric muscle contractions, and maximal or submaximal concentric muscle contractions [14, 15]. Overuse injuries are prevalent among high school and other athletes [16]. Muscle injuries represent 10% to 55% of all injuries in sports [17], commonly treated with thermal modalities, massage, or external devices, such as a foam roller. Muscle overload is one of the precursors of the development of trigger points, which can lead to muscle weakness [18], fatigue [19], and restricted movement [20, 21], affecting an athlete’s performance [22]. As a side note, none of these parameters can be used to detect trigger points specifically. The performance of athletes can be significantly impacted by the presence of trigger points [22, 23].
Although there is not much research on the value of dry needling for injury prevention, there is much evidence that dry needling can contribute to increased performance [12, 21, 24, 25], recovery [26-29], and treatment of athletic injuries [22, 29-31]. Athletic trainers can play a significant role in the well-being of athletes when they include dry needling.
Myopain Seminars Dry Needling Courses by Athletic Trainers
Myopain Seminars offers a dry needling course series designed for athletic trainers. Any athletic trainer interested in enhancing their client’s athletic performance should add dry needling to their toolbox. Of course, Myopain Seminars is the obvious choice!
Todd Hooks PT, ATC, OCS, SCS, MOMT, MTC, CSCS, CMTPT, NREMT-1, FAAOMPT
Dry Needling of Athletes Course Series
The Dry Needling of Athletes-1 course is designed to incorporate dry needling in the overall care of athletes and is particularly suited for athletic trainers and physical therapists with an athletic patient population. Myopain Seminars is an approved BOC course provider (P8248).
The Dry Needling of Athletes- 2 course builds on the knowledge and skills of the DN-AT 1 course. The course will bring the ATC and PT to the highest level of clinical proficiency in managing athletes with myofascial pain, preparing students for the final practical examinations leading to the CMTPT/DN-AT qualification!
Coming soon
The Dry Needling of Athletes; Advanced course is designed as a post-certification course and covers muscles in the chest and craniomandibular regions. Furthermore, the course addresses more advanced dry needling approaches bringing the ATC and sports PT to the highest level of proficiency. Coming soon!
References
1. Caramagno, J., et al., Analysis of competencies for dry needling by physical therapists. 2015, Federation of State Boards of Physical Therapy: Alexandria.
2. Soyring, K. Dry Needling by Occupational Therapists. 2021 [cited 2022 August 15].
3. Cummings, M., Dry needling from a western medical acupuncture perspective, in Trigger point dry needling; an evidenced and clinical-based approach, J. Dommerholt and C. Fernández de las Peñas, Editors. 2013, Churchill Livingstone: Edinburgh. p. 173-207.
4. Chiropractors Registration Board Of Victoria, Guidelines For The Practice Of Acupuncture And Dry Needling By Chiropractors. 2005, Chiropractors Registration Board Of Victoria: Melbourne.
5. Graff-Radford, B., Myofascial trigger points: their importance and diagnosis in the dental office. J Dent Assoc S Afr, 1984. 39(4): p. 249-53.
6. Wall, R., Introduction to Myofascial Trigger Points in Dogs. Top Companion Anim Med, 2014. 29(2): p. 43-48.
7. Hortz, B.V., S. Falsone, and D. Tulimieri, Current Athletic Training Educational Preparation for Dry Needling. J Sports Med Allied Health Sci, 2019. 4(3): p. 5.
8. AT Strategic Alliance. Strategic Alliance Degree Statement. 2015 [cited 2022 August 15]
9. Commission on Accreditation of Athletic Training Education. (2018). 2020 Standards for the Accreditation of Professional Athletic Training Degree Programs. Austin, TX
10. National Athletic Trainers’ Association. (2011). Athletic Training Education Competencies. Dallas, TX
11. National Athletic Trainers’ Association. Dry Needling in Athletic Training. [cited 2022 August 15]
12. Tang, C.T. and B. Song, Acupuncture and Dry Needling for Sports Performance and Recovery. Curr Sports Med Rep, 2022. 21(6): p. 213-218.
13. Kamali, F., et al., Dry needling versus friction massage to treat tension type headache: A randomized clinical trial. J Bodyw Mov Ther, 2019. 23(1): p. 89-93.
14. Bron, C. and J. Dommerholt, Etiology of myofascial trigger points. Curr Pain Headache Rep, 2012. 16(5): p. 439-44.
15. Hamlin, M.J. and B.M. Quigley, Quadriceps concentric and eccentric exercise 2: differences in muscle strength, fatigue and EMG activity in eccentrically-exercised sore and non-sore muscles. J Sci Med Sport, 2001. 4(1): p. 104-15.
16. Schroeder, A.N., et al., Epidemiology of overuse injuries among high-school athletes in the United States. J Pediatr, 2015. 166(3): p. 600-6.
17. Jarvinen, T.A., et al., Muscle injuries: biology and treatment. Am J Sports Med, 2005. 33(5): p. 745-64.
18. Bagcier, F., et al., The relationship between gluteus medius latent trigger point and muscle strength in healthy subjects. J Bodyw Mov Ther, 2022. 29: p. 140-145.
19. Ge, H.Y., L. Arendt-Nielsen, and P. Madeleine, Accelerated muscle fatigability of latent myofascial trigger points in humans. Pain Med, 2012. 13(7): p. 957-64.
20. Wilke, J., et al., Range of motion and cervical myofascial pain. J Bodyw Mov Ther, 2016. 20(1): p. 52-5.
21. Haser, C., et al., Effect of Dry Needling on Thigh Muscle Strength and Hip Flexion in Elite Soccer Players. Med Sci Sports Exerc, 2017. 49(2): p. 378-383.
22. Osborne, N.J. and I.T. Gatt, Management of shoulder injuries using dry needling in elite volleyball players. Acupunct Med, 2010. 28(1): p. 42-45.
23. Ortega-Santiago, R., et al., Pressure pain hypersensitivity and referred pain from muscle trigger points in elite male wheelchair basketball players. Braz J Phys Ther, 2019.
24. Bandy, W.D., R. Nelson, and L. Beamer, Comparison of Dry Needling Vs. Sham on the Performance of Vertical Jump. Int J Sports Phys Ther, 2017. 12(5): p. 747-751.
25. Janowski, J.A., et al., Acute Effects of Dry Needling on Myofascial Trigger Points in the Triceps Surae of Ballet Dancers: A Pilot Randomized Controlled Trial. Int J Sports Phys Ther, 2021. 16(2): p. 418-430.
26. Ershad, N., et al., The effects of dry needling as a novel recovery strategy on quadriceps muscle fatigue: A pilot study. Journal of Iranian Medical Council, 2019. 2(6): p. 215-221.
27. Brewster, B.D., A.R.S. Valier, and S. Falsone, A Systematic Dry Needling Treatment Supports Recovery Post-Training for Division I Ice Hockey Athletes: An Exploration Case Series. J Athl Train, 2021.
28. Thompson, R., M. Prosell, and T. Timpka, Elite athletes’ experiences of musculoskeletal pain management using neuroanatomical dry needling: A qualitative study in Swedish track and field. J Sci Med Sport, 2021. 24(1): p. 46-51.
29. Lopez-Gonzalez, L., et al., Effects of Dry Needling on Neuromuscular Control of Ankle Stabilizer Muscles and Center of Pressure Displacement in Basketball Players with Chronic Ankle Instability: A Single-Blinded Randomized Controlled Trial. Int J Environ Res Public Health, 2021. 18(4).
30. Gonzalez-Iglesias, J., et al., Multimodal management of lateral epicondylalgia in rock climbers: a prospective case series. J Manipulative Physiol Ther, 2011. 34(9): p. 635-42.
31. Paantjens, M.A., Dry needling en adductorenmanipulatie voor de behandeling van een voetballer met adductorgerelateerde liespijn. Ned Mil Genees Tijdschr, 2013. 66–61–68: p. 64-70.