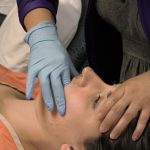
The American Physical Therapy Association (APTA) defines dry needling (DN) as “a skilled intervention utilized by physical therapists that uses a thin filiform needle to penetrate the skin and stimulate underlying myofascial trigger points, muscular, and connective tissues for the management of neuromusculoskeletal pain and movement impairments” (1).
Typically, dry needling is performed to target myofascial trigger points in muscle and is based on the work of Janet Travell, MD, David Simons, MD, and others (2); however, in recent years, techniques have evolved to also target tendon, fascia, and scar tissue (3). Dry needling techniques performed by physical therapists are different in both theory and practice from techniques performed by acupuncturists (1). Although the APTA defines dry needling as within the scope of PT practice, regulations vary by state and PTs are not allowed to practice dry needling in all states (4). Physical therapists are responsible for knowing the rules and laws in the state in which they practice.
A trigger point (TrP) is a discrete and palpable nodule within a taut band of muscle that is exquisitely tender with mechanical stimulation (5). The pain from a myofascial trigger point may remain local or may refer to a different and remote part of the body. Trigger points may develop in muscle for a variety of reasons, including, but not limited to trauma, concentric muscle overload, eccentric muscle overload, prolonged postural overload, and repetitive low-load muscle activity (5). With various constructs of muscle overload, an energy crisis occurs. Blood flow to the muscle fibers is restricted, causing a back-up or retrograde blood blow. This results in ischemia, decreased oxygenation to the tissue, and a lowering of pH, resulting in an acidic environment. This acidic environment results in a chemical cascade that will change the thresholds and permeability of specific nociceptors. We know from in-vivo microdialysis of the area in and around the trigger point that concentrations of specific nociceptive chemicals are higher inside a myofascial trigger point, including adenosine triphosphate (ATP), bradykinin (BK), 5-hydroxy- tryptamine (5-HT, serotonin), prostaglandins, and potassium (K+) (6). We also know that electrical activity is increased near a trigger point, resulting in motor endplate noise (7).
Trigger points may result in impairments including pain, range of motion restrictions, muscle inhibition, and changes in muscle activation patterns and motor control (8). Any and all of these impairments may be addressed by treating the trigger points with dry needling. Historically, trigger points were treated by injection of various substances using a hypodermic needle. Current research demonstrates that dry needling, or the use of a small filiform needle, is as effective or more effective than trigger point injections, without the potential side effects that may occur with medications commonly used with TrP injections (9).
Although there is a paucity of research on the topic, dry needling is also being used to address tendinopathy and scar tissue with a variety of needle manipulations including pistoning and rotating.
Current research hypothesizes that the mechanism for the effect is due to mechanical transduction signaling through connective tissue (10). Pistoning of the needle may also stimulate blood flow to the area to allow a re-initiation of the inflammatory and healing processes.
There is very little research available on the treatment of trigger points in performing artists. There are, however, several articles published recognizing that myofascial pain can be present in performing artists, particularly in the head, neck and upper extremities of vocalists and musicians (11, 12).
Performing arts medicine – Instrumentalist musicians: Part III – Case histories
These authors note that myofascial pain syndromes may mimic other neuromusculoskeletal diagnoses such as carpal tunnel syndrome, TMJ pathology, migraine headache, DeQuervan’s tenosynovitis, arthritis, and ulnar nerve pathology, to name a few. For example, an ill-fitting string instrument may lead to compensations in the upper extremity that result in significant overload to extensor carpi radialis longus muscle and infraspinatus muscle, which could result in myofascial pain that imitates the pain complaints of DeQuervain’s tenosynovitis (2).
T![]() here is less literature to support the existence of myofascial pain syndromes and the use of dry needling in the lower extremities in performing artists; however, in treating performing artists, we often see patients with complaints of heel pain and “plantar fasciitis.” Clinicians should be aware of the contributing factors of muscle referred pain patterns in these diagnoses. For example, there are multiple muscles whose referral pattern mimics a plantar fasciitis-type pain: gastroc, soleus, flexor digitorum longus, quadratus plantae, abductor hallucis, and tibialis posterior (2, 13).
here is less literature to support the existence of myofascial pain syndromes and the use of dry needling in the lower extremities in performing artists; however, in treating performing artists, we often see patients with complaints of heel pain and “plantar fasciitis.” Clinicians should be aware of the contributing factors of muscle referred pain patterns in these diagnoses. For example, there are multiple muscles whose referral pattern mimics a plantar fasciitis-type pain: gastroc, soleus, flexor digitorum longus, quadratus plantae, abductor hallucis, and tibialis posterior (2, 13).
All of these muscles should be examined for myofascial trigger points in addition to the typical orthopedic exam including active and passive range of motion, strength testing, selective tissue tensioning, special tests, posture, and alignment, etc. Clinicians are beginning to get more case reports in the literature regarding the use of dry needling in treating dancers (14). Clinicians should be encouraged to contribute to evidence-based practice in this valuable way.
In all performing artists, it is important to look at the patient performing their specific task. Whether it is the posture and fingering of a violinist or relevé and landing mechanics of a classical ballerina, clinicians can gain important information regarding repetitive loading, sustained postural loads and muscle imbalances that may be contributing factors to the development of trigger points and myofascial pain syndromes.

A classic example is a violinist suffering from tension-type headaches because of sustained cervical rotation that is causing trigger points in the suboccipital muscles or sternocleidomastoid muscle (SCM). In this case, bilateral SCMs, the suboccipitals, as well as the posterior cervical muscles and deep cervical flexors will need to be examined. Is the dancer forcing turnout, overusing deep hip rotators, inhibiting the gluteal muscles, leading to increased valgus stress at the knee with landing jumps? In such a presentation, it would be important to examine and treat trigger points in the deep rotator muscles, gluteal muscles, adductor muscles, and quadriceps muscle groups. In these cases, trigger points are a contributing factor to the pain complaints and must be addressed in addition to accessory joint motion, postural and motor control impairments.
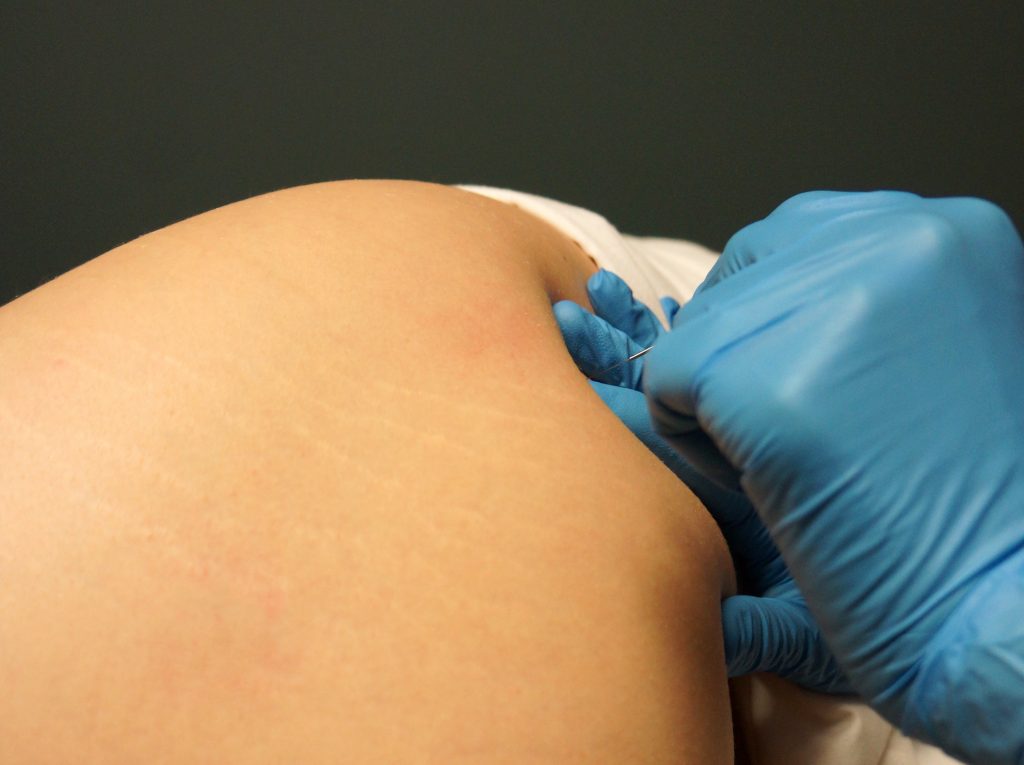
Trigger points may also present as a result of acute injury. In the case of a dancer presenting with a lateral ankle sprain due to a plantarflexed and inverted landing, the fibularis longus and brevis muscles may also respond with trigger points due to eccentric overload sustained during the injury. These trigger points may be the cause of persistent lateral ankle pain. In the case of an acute hamstring strain, the patient may present with trigger points in conjunction with swelling, range of motion and strength impairments. If a dancer sustains a concussion and a whiplash injury during a performance, she may also present with trigger points in the sternocleidomastoid, deep cervical flexors, upper trapezius, suboccipital and splenius capitus muscles.
Practitioners should keep in mind that trigger points can also be effectively treated without the invasive intervention of dry needling. If the PT is practicing in a state whose practice act does not allow for the use of needles, it is important to learn manual assessment and treatment techniques for trigger points. Sustained compression, with or without repeated contractions, may be used to treat most muscles in the body. There are also muscles in which dry needling may be a precaution or contraindication for a variety of reasons. For example, Myopain Seminars does not teach dry needling of the posterior tibialis muscles secondary to anatomic anomalies seen in the neurovascular structures in the deep posterior compartment. We believe that needling this muscle may increase the risk of bleeding and compartment syndromes. Precaution should always be taken in needling patients on anticoagulant therapy; however, needling muscles in which direct hemostasis cannot be applied, i.e. lateral pterygoid and psoas, would be a contraindication with increased risk of bleeding. In the case of pregnancy, needling in the first trimester and in and around the abdominal wall, lumbar spine and pelvis may be discouraged. Localized or systemic infection, metastasis, breast or pectoral implants, communication barriers, and fear of needles are other examples of cases in which manual treatment of trigger points may be used. In the case of a performing artist, dry needling may be avoided 24-48 hours prior to performance due to the potential for residual soreness and alterations in muscle firing and patterning. This is determined on a case-by-case basis and the patient’s prior response to dry needling should always be considered.

As the physical therapy provider for a professional ballet company, I use dry needling frequently as part of holistic care for the performers. It is our experience that the dancers tolerate and respond very well to the intervention. In general, they are extremely aware of their bodies and notice even the slightest restriction in range of motion, strength, and ability to stabilize. From experience, most of the dancers prefer to be treated with needles at the end of their workday or even workweek so that they have time to recover. It is extremely rare that we provide dry needling interventions on a dancer on the day of the performance. As with any intervention, dry needling and trigger point treatment must always be used in conjunction with other manual therapies, therapeutic exercises, and neuromuscular re-education as appropriate.
Mandy Blackmon PT, DPT, OCS, CMTPT is the primary physical therapy provider for the Atlanta Ballet. She is on faculty in the entry-level PT program at Mercer University and is an instructor for Myopain Seminars’ Dry Needling courses.
References
- American Physical Therapy Association. Physical therapists & the performance of dry needling: An educational resource paper, 2012. Alexandria, VA.
- Simons, DG, Travell JG, Simons, LS. Travell and Simons’ myofascial pain and dysfunction: the trigger point manual. Volume 1. The upper half of the body. 2nd ed. Baltimore, MD: Williams & Wilkins; 1999.
- Krey D, Borchers J, McCamey K. Tendon needling for treatment of tendinopathy: A systematic review. The Physician And Sportsmedicine. 20015;43(1): 80-86.
- Myopain Seminars. Resources: Dry Needling Rulings 2016. Accessed August 10, 2016.
- Gerwin RD, Dommerholt J, et al. An expansion of Simons’ integrated hypothesis of trigger point formation. Current Pain Headache Reports. 2004;8(6): 468-475.
- Shah JP, Gilliams EA. Uncovering the biochemical milieu of myofascial trigger points using in vivo microdialysis: an application of muscle pain concepts to myofascial pain syndrome. J Bodywork Movement Therapies. 2008;12(4): 371-384.
- Ge HY, Zhang Y, et al. Induction of muscle cramps by nociceptive stimulation of latent myofascial trigger points. Exp Brain Res. 2008;187(4): 623-629.
- Lucas KR, Rich PA, et al. Muscle activation patterns in the scapular positioning muscles during loaded scapular plane elevation: the effects of Latent Myofascial Trigger Points. Clin Biomech. 2010; 25(8): 765-770
- Ga H, Koh HJ, et al. Intramuscular and nerve root stimulation vs lidocaine injection to trigger points in myofascial pain syndrome. J Rehabil Med: 2007;39(5): 374-378
- Langevin HM, Churchill DL, Fox JR, Badger GJ, Garra BS, Krag MH. Biomechanical response to acupuncture needling in humans. J Appl Physiol/./2001;91(6):2471-2478
- Rosen NB. Myofascial pain: the great mimicker and potentiator of other diseases in the performing artist. Maryland Med J. 1993;42(3): 261-266.
- Dommerholt J. Performing arts medicine – instrumentalist musicians: part III – case histories. J Bodyw Mov Ther . 2010;14(2): 127-138.
- Cotchett, M. P., K. B. Landorf, et al. “Effectiveness of dry needling and injections of myofascial trigger points associated with plantar heel pain: a systematic review.” Journal of foot and ankle research. 2010;3:18.
- Mason JS, Tansey KA, Westrick RB. Treatment of subacute posterior knee pain in an adolescent ballet dancer utilizing trigger point dry needling: A case report. 2014; 9(1): 116-124.