Knee Pain in Runners: A Common Affliction
So much of life bounces in the grey area of “maybe.” There is, however, one sure thing that isn’t in the grey: runners are going to run. If you treat runners, you know this. If you are a runner, you know this. The protracted history of this young lady’s efforts to run without symptoms is illustrative. She struggled with how to solve knee pain from running—running and knee pain aren’t an odd combination, especially kneecap area pain, as it makes up 15-25% of all knee pain complaints.
The Emergence of Knee Pain in a Young Woman Runner
This young woman, let’s call her Tia, ran competitively in high school and college with a not atypical history of several non-serious, over-use lower extremity injuries. But after college, she developed knee pain due to running unlike any she had previously encountered.
Tightness Around Patella With Ache Behind Knee Cap
While transitioning her programming between running and biking, she developed symptoms around her right patella area. She wasn’t feeling a sharp knee pain from running, but more of a “tightness” around her patella. It wasn’t so much front knee pain but more an ache behind her knee cap. She could not relieve her symptoms consistently or substantially with ice and a reduction or even temporary cessation of running. She resumed reduced running and biking. She sought help from her physical therapist and began to do patella-femoral arthralgia (PFA) therapeutic exercises. This initial treatment also included dry needling for knee pain in her quadriceps and gluteal muscles. She had some initial improvement, but her progress was short-lived as symptoms continued to re-surface after runs.
Custom Orthotics, Chiropractic Manipulation, and a Suggestion for Diagnostic Arthroscopy
Over a 24-month orthopedic odyssey, she would go on to new physical therapy exercises for knee pain (a second physical therapist), two sets of custom orthotics, a few months of chiropractic manipulation, an orthopedic consultation, x-rays, and an MRI. She had, after this, a veritable dossier of therapeutic exercises but no real relief. In fact, her symptoms now had begun to radiate proximally from her patella to the mid-thigh.
At this time, Tia’s orthopedic surgeon physician suggested a diagnostic arthroscopy for further treatment. Wanting to avoid surgery, she called her “old” PT from her high school days (me) and asked if I would examine her to see if there was something or some way I could help. I agreed to have a look, and she traveled the 328 miles for a visit.
Examining the Runner’s Knee Pain
Tia walked in without an apparent gait anomaly or obvious pain and presented her well-worn loose-leaf notebook collection of leg, hip, and core exercises.
Initial Assessment: Peri-Patellar Tightness That Radiated to the Thigh From Running
I found myself in the enviable position of having slightly longer than a 2-year history of assessment and treatment by podiatry, physical therapy, chiropractic, and medical professionals. This afforded me some liberty because my evaluation didn’t need to include the typical meniscal or medical screening concerns per se, for instance.
At the time of the evaluation, Tia was a 26-years old fit individual with very low body fat. She complained of peri-patellar tightness/ache that radiated proximally to the mid-thigh with and after running. This pain occurred within the first mile of running but didn’t seem to worsen through the run.
Lumbar Scan, Muscle Tests, and Movement Assessments
We performed a brief lumbar scan with DTR (2+ bilaterally at patella and Achilles), normal myotomal L2-S1 key muscle tests, and cardinal plane torso movement assessment. These were mainly unremarkable and WNL except for a very slight lumbar scoliosis, concave right.
She had a slight gait anomaly due to this curve as her trunk deviated slightly toward her right side with right leg heel strike and foot flat (this has been associated with knee pain in females after running). She had a medium-height arch with good re-supination at heel off. Her orthotics matched her foot contours and visually helped control her calcaneus standing with extrinsic rearfoot posting and what seemed to be intrinsic forefoot posting. Since this was her second pair and she had extensive workup via her podiatrist, I deferred any extensive subtalar joint/foot assessment.
Her knee was without obvious inflammatory signs: no swelling, no extra warmth, and normal skin color. She had equal and total knee ROM: 5-0-140 bilaterally and had full muscle length tests for hamstrings, quadriceps, calf (with the knee flexed and extended), and hip flexors. Her Thomas test was unremarkable, with her limb hanging in rotational neutral at 80 degrees of knee flexion with her thigh level to the exam table. She had hip rotation, abduction, and adduction within normal limits bilaterally.
Sensory testing was deferred. No visual excessive patellar tilt was noted bilaterally. However, since one provider had mentioned she had patella alta on the right, patellar tendon length from the tibial tubercle to the inferior pole was measured and found bilaterally equal.
Muscular Testing and Palpation of Patellar Facets
Palpation of patellar facets did not reproduce pain or crepitus. The grind test was not performed since the MRI was negative for chondral involvement, and the test has shown poor diagnostic validity. Ligament stress tests were stable. As mentioned previously, meniscal tests were not performed. Manual muscle testing of her knee extension, flexion, and abduction were all 5/5 without pain. The step-down test was stable without deviation in speed or from the sagittal plane but with a “tightness” peri-patellar on the right. I began to think more about a muscular source of pain since I could not provoke any symptoms to this point and her symptom complaint was of “aching,” which is a more common complaint with muscle-sourced pain, and tightness.
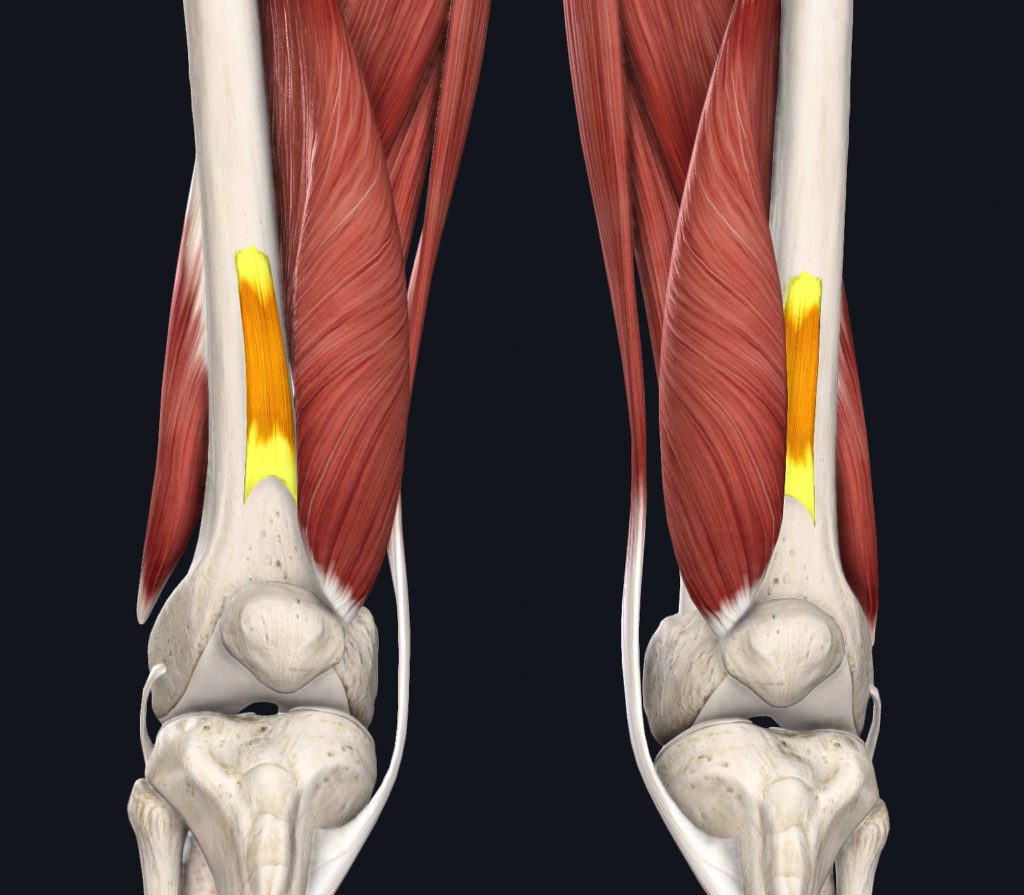
Palpation of Calf and Anterior and Medial Thigh Musculature
Extensive palpation of her anterior and medial thigh musculature and her calf were performed, and I was able to reproduce a portion of her symptoms with prolonged palpation on an area approximately 3 inches proximal to her patella over her anterior thigh. This is over the belly of the articularis genu or more commonly called genu articularis muscle and distal rectus femoris tendon. If this muscle is news to you, don’t be embarrassed as many long-established clinicians have never heard of it either, and for a good reason, as it’s probably not a frequent producer of symptoms and has no established pain referral pattern. It’s a small muscle on the anterior distal femur surface, deep to the rectus femoris tendon. It attaches to the superior edge of the synovium and suprapatellar bursa and functions to tense these tissues during knee extension, essentially pulling them clear of the patella. She also had latent myofascial trigger points in her vastus lateralis, but palpation here did not replicate any of her symptoms.
Myofascial Trigger Point Treatment
Since she had so much previous work done via therapeutic exercise techniques and foot assessment, I focused exclusively on her myofascial trigger points. Since I could reproduce some of her symptoms via the genu articularis, I directed my attention there.
Dry Needling the Genu Articularis
Tia had already had dry needling for knee pain from one of her previous therapists (not Myopain Seminars trained, however). Still, only the quadriceps and gluteals were needled, not the genu articularis.
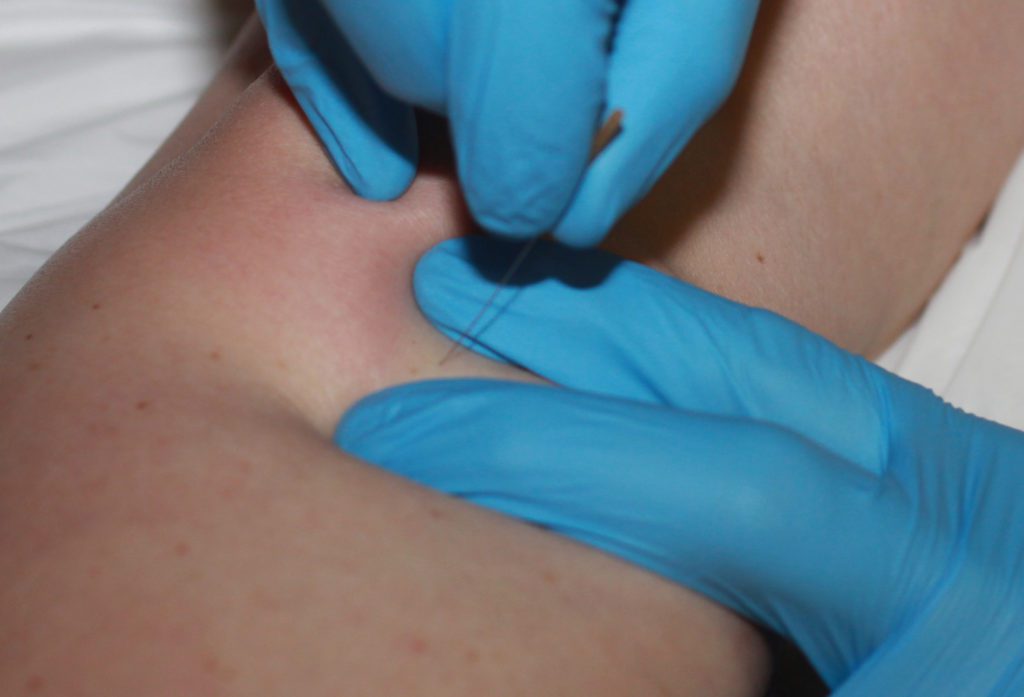 I needled the genu articularis in accordance with Myopain Seminars instructed technique and the text “Trigger point dry needling: An Evidence and Clinical-Based Approach,” 2nd ed by Dommerholt and Fernández-de-las-Peñas. The needling created a local twitch response and reproduced her retro-patellar ache; when twitches were no longer provoked, soft tissue therapeutic massage was used over the distal anterior thigh followed by a 30-second stretch of her quadriceps. Since she had the lateral quad previously needled, I wanted to see the particular benefit of only treating the articularis genu.
I needled the genu articularis in accordance with Myopain Seminars instructed technique and the text “Trigger point dry needling: An Evidence and Clinical-Based Approach,” 2nd ed by Dommerholt and Fernández-de-las-Peñas. The needling created a local twitch response and reproduced her retro-patellar ache; when twitches were no longer provoked, soft tissue therapeutic massage was used over the distal anterior thigh followed by a 30-second stretch of her quadriceps. Since she had the lateral quad previously needled, I wanted to see the particular benefit of only treating the articularis genu.
Symptom-Free Running After Dry Needling
Since her symptoms were easily provoked with nearly any running, I asked her to run on the treadmill to check her symptoms. She reported an approximate 85% improvement immediately. I asked her to use self-massage, stretching, and continued use of her therapeutic program until she could follow up with her home therapist.
I contacted her home PT and described the anatomy and technique of needling the genu articularis (as the course work for her dry needle education did not include this muscle) for follow-up care and had my own follow-up three weeks later. Tia reported her symptoms had significantly improved after another two sessions with her other PT, and she was enjoying symptom-free running again after a 2-year journey.
Long-Term Results: Occasional Dry Needling of the Genu Articularis
As a long-term follow-up, I contacted Tia 5 years later. For most of the year, she is without symptoms. She has found a symptom-production pattern when she transitions from running to more biking in the spring. She can feel “her” symptom coming back, but she can eliminate it with the occasional dry needle of her genu articularis. So, does dry needling help a runner’s knee? Tia and I would both say a hearty “yes!”
Ralph Simpson PT, DPT, OCS, CMPT, CMTPT, LATC
Sources:
Lankhorst NE Bierma-Zeinstra SM van Middelkoop M. Risk factors for patellofemoral pain syndrome: a systematic review. J Orthop Sports Phys Ther. 2012;42(2):81-94.
Ahmed CS McCarthy M Gomez JA, et al. The moving patellar apprehension test for lateral patellar instability. Am J Sports Med 2009;37:791-796.
Nunes GS Stapait EL Kirsten MH de Noronha M Sanatos GM. Clinical test for diagnosis of patellofemoral pain syndrome: systematic review with meta-analysis. Phys Ther Sport. 2013;14(1):54-59.
Post WR Fulkerson J. Knee pain diagrams: correlation with physical examination findings in patients with anterior knee pain. Arthroscopy 1984;10(6):618-623.
Pappas E Wong-Tom WM. Prospective predictors of patellofemoral pain syndrome: A systematic review with meta-analysis. Sports Health. 2012;4(2):115-120.
Nakagawa TH Moriya ETU Maciel CD Serrao FV. Trunk, pelvis, hip, and knee kinematics, hip strength, and gluteal muscle activation during a single-leg squat in males and females with and without patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2012;42(6):491-501.
Ugalde V Brockman C Bailowitz Z Pollard CD. Single leg squat test and its relationship to dynamic knee valgus and injury risk screening. Phys Med Rehabil. 2015;7(3):229-235; quiz 235.
Loudon JK Wiesner D Goist-Foley HL Asjes C Loudon KL. Intrarater reliability of functional performance tests for subjects with patellofemoral pain syndrome. J Athl Train. 2002;37(3):256-261.
Lee SP Souza RB Powers CM. The influence of hip abductor muscle performance on dynamic postural stability in females with patellofemoral pain. Gait Posture. 2012;36(3):425-429.
Levinger P Gilleard W Coleman C. Femoral medial deviation angle during a one-leg squat test in individuals with patellofemoral pain syndrome. Phys Ther Sport. 2007;8(4):163-168.
Standring S. Gray’s Anatomy: The Anatomical Basis of Clinical Practice. 41st ed. London, UK: Elsevier; 2015.
Willett GM Keim S Shostrom VK Lomneth CS. An Anatomic Investigation of the Ober Test. Am J Sports Med. 2016;Mar;44(3):696-701
Doberstein ST Romeyn RL Reineke DM. The Diagnostic Value of the Clarke Sign in Assessing Chondromalacia Patella. J Athl Train. 2008 Mar-Apr; 43(2): 190-196.
Cover photo by Andrew Tanglao on Unsplash