The Physical and Mental Impacts on Athletes
The physical and mental demands of physical training and competing in sporting activities can be stressful and taxing to athletes of all levels. Sport participation has become a year-round activity, with young athletes involved in the same sport without having an off-season to allow the body to recover from the stresses and strains imposed. The role of the rehabilitation specialist in sports medicine has become more valued as greater demands on training and competition are placed on athletes at all levels. As a result of the increased pressure of competition and the expectations of excelling, athletes are often regulated to participate and train in a single sport. Sports-specialized training places athletes at a higher risk of injury because of over-use, repetitive activity, and year-round training (Myer et al., 2015).
A media content analysis revealed that over 72% of elite tennis players suffered from injury-related problems compared to about 27% of amateur players (Musa et al., 2022). Muscle injuries range from 10% to 55% of all sporting injuries and may have the highest incidence in sports (Ruf et al., 2022).
Repetitive stresses are abundant as athletes continually train to improve strength, endurance, and agility. Athletic competition can also tax athletes as the stresses generated and imposed can cause soft tissue injuries. Lastly, athletes’ mental stresses (both internal and external) can affect their ability to perform and recover.
Trigger Points in Athletes
Trigger points are commonly found in many different kinds of athletes, including elite swimmers (Hidalgo-Lozano et al., 2010; Hidalgo-Lozano et al., 2013), baseball players (Chiu et al., 2020), track and field athletes (Thompson et al., 2021), professional basketball players (Yeste-Fabregat et al., 2021) and wheelchair basketball players (Ortega-Santiago et al., 2019), runners (Jungmalm et al., 2020), ice hockey players (Brewster et al., 2021), overhead athletes (Kamali et al., 2019), soccer players (Paantjens, 2013), professional volleyball players (Osborne & Gatt, 2010), and handball players (Ceballos-Laita et al., 2021), among others.
Rehabilitation Technique for Athletes: Dry Needling
Athletes at all levels rely upon medical staff personnel to provide care and treatment for their injuries and aid recovery. Dry needling therapy is a relatively new rehabilitation technique for athletes. As the demands for athletes have increased, so have the demands for rehabilitation techniques for sports medicine and athletic training. Dry needling (DN) by athletic trainers and sports physical therapists is performed to augment recovery, prevent injury, and enhance performance.
Examples of Dry Needling Treatment for Sport Injuries
Trigger Points (TrPs) can develop in athletes due to muscle overload, overuse, repetitive activity, and excessive eccentric muscle activity (Gerwin, 2008). Dry needling affects the biomechanical (Langevin et al., 2006), chemical (Shah et al., 2008), and vascular (Larsson et al., 1999) properties of soft tissue. Also, DN is more effective in improving pressure pain thresholds than manual TrP therapy (Llamas-Ramos et al., 2014). Patients with unilateral ankle instability that received DN into the lateral fibularis muscle along with proprioception and strengthening exercises have improved outcomes in both pain and outcome functional measurements compared to those receiving exercise training alone (Salom-Moreno et al., 2015). Tendinopathy can be debilitating in athletes, as a lack of blood flow and ensuing a hypoxic tissue environment can lead to pain and disability. Dry needling has been advocated in managing tendinopathy as it has been shown to increase blood flow via local vasodilation (Kubo et al., 2010; James et al., 2007) and collagen proliferation (Langevin et al., 2007).
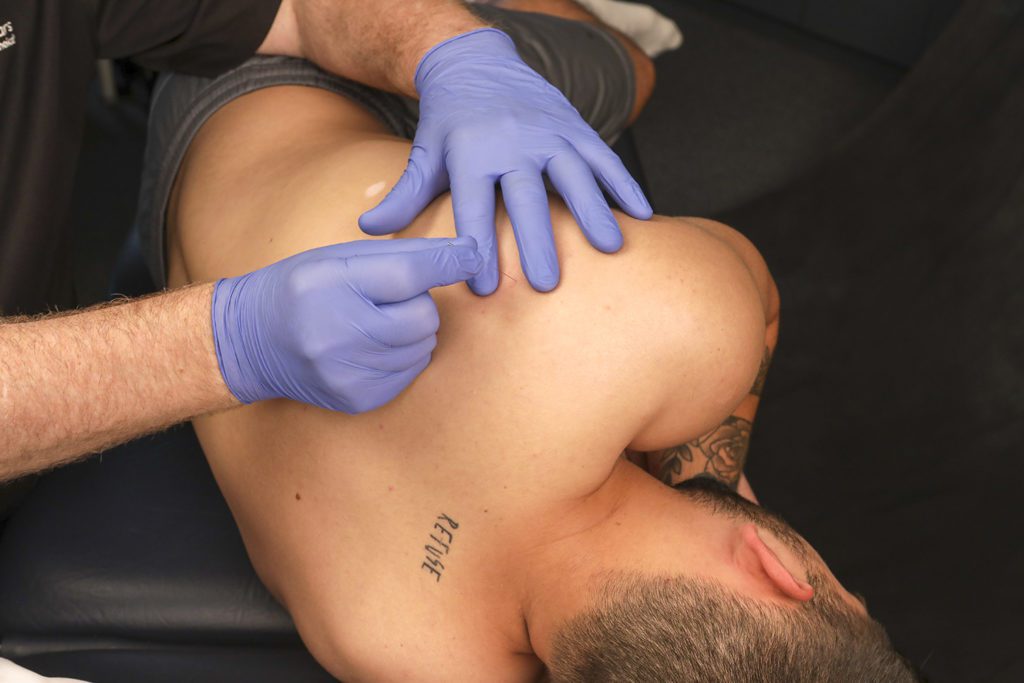 Osborne and Gatt (2010) revealed improved shoulder range of motion, function, and decreased pain in elite volleyball players receiving DN to the scapulohumeral musculature during the season. Dry needling in subjects with supraspinatus tendon lesions (tendinosis or partial tear) has been shown to have improved outcome measures and shoulder range of motion (Rha et al., 2013). Posterior shoulder tightness is a common finding in overhead athletes, for which stretching, massage, and joint mobilizations are often utilized in treatment. Passigli and coworkers (2016) demonstrated using DN to the infraspinatus, teres minor, and posterior deltoid muscles to improve shoulder horizontal adduction and internal rotation range of motion and decrease pain reproduction. Dry needling followed by active stretching is more effective than stretching alone, which could lead to increased TrP sensitivity (Decoster et al., 2005).
Osborne and Gatt (2010) revealed improved shoulder range of motion, function, and decreased pain in elite volleyball players receiving DN to the scapulohumeral musculature during the season. Dry needling in subjects with supraspinatus tendon lesions (tendinosis or partial tear) has been shown to have improved outcome measures and shoulder range of motion (Rha et al., 2013). Posterior shoulder tightness is a common finding in overhead athletes, for which stretching, massage, and joint mobilizations are often utilized in treatment. Passigli and coworkers (2016) demonstrated using DN to the infraspinatus, teres minor, and posterior deltoid muscles to improve shoulder horizontal adduction and internal rotation range of motion and decrease pain reproduction. Dry needling followed by active stretching is more effective than stretching alone, which could lead to increased TrP sensitivity (Decoster et al., 2005).
Dry needling has increased maximal endurance and force in knee extensor muscles in elite soccer players (Haser et al., 2017). Another study showed that DN improved hamstrings flexibility (Alaei et al., 2021). Bandy et al. (2017) demonstrated a significant increase in vertical jump following one session of dry needling in a group of healthy subjects as compared to sham dry needling. TrPs have been shown to accelerate muscle fatigue and tax neighboring motor units to the TrP (Ge et al., 2012). Eliminating the TrP can reduce augmented muscle fatigue and help reduce potential overload within the muscle (Ge et al., 2012).
extensor muscles in elite soccer players (Haser et al., 2017). Another study showed that DN improved hamstrings flexibility (Alaei et al., 2021). Bandy et al. (2017) demonstrated a significant increase in vertical jump following one session of dry needling in a group of healthy subjects as compared to sham dry needling. TrPs have been shown to accelerate muscle fatigue and tax neighboring motor units to the TrP (Ge et al., 2012). Eliminating the TrP can reduce augmented muscle fatigue and help reduce potential overload within the muscle (Ge et al., 2012).  Ershad et al. (2019) showed that DN can be used as a novel recovery strategy for quadriceps muscle fatigue. Athletes can also suffer psychological stresses from competition and non-competition sources (Noblet and Gifford, 2007). Psychological stressors can decrease the rate of strength recovery from strength workouts (Stults-Kolehmainen and Bartholomew, 2012). Dry needling can influence the anterior cingulate cortex and limbic system (Hui et al., 2000; Wu et al., 2002), which could affect frequent emotional stresses in athletics.
Ershad et al. (2019) showed that DN can be used as a novel recovery strategy for quadriceps muscle fatigue. Athletes can also suffer psychological stresses from competition and non-competition sources (Noblet and Gifford, 2007). Psychological stressors can decrease the rate of strength recovery from strength workouts (Stults-Kolehmainen and Bartholomew, 2012). Dry needling can influence the anterior cingulate cortex and limbic system (Hui et al., 2000; Wu et al., 2002), which could affect frequent emotional stresses in athletics.
Dry Needling Is an Effective Option for Athletes
Athletes seek professional care in providing daily maintenance and rehabilitation following injury. Dry needling is a treatment technique that can be utilized in the care of athletes that provides many benefits. In addition to augmenting local tissue recovery, DN has been shown to release opioid peptides, reduce the nociceptive input from the TrP, and therefore decrease the overall pain and sensitivity that accompanies TrPs (Lavelle et al., 2007; Ge et al., 2009; Affaitati et al., 2011). While the use of opioids in athletics is well documented (Ekhtiari et al., 2020), practitioners need to offer alternative options that provide effective care aimed at both restoring function and decreasing the pain that often accompanies sports.
Dry needling is a treatment technique that can aid athletes in pursuing training and competing in their sporting activity. As physical therapists and athletic trainers seek to expand their treatment skills through continuing education, DN can be an effective treatment modality to aid an athlete in returning to play.
Todd Hooks, PT, ATC, OCS, SCS, FAAOMPT
Jan Dommerholt, PT, DPT
References
- Affaitati G, Costantini R, Fabrizio A, Lapenna D, Tafuri E, Giamberardino MA. 2011. Effects of treatment of peripheral pain generators in fibromyalgia patients. Eur J Pain. 15:61-69.
- Alaei, P, Ansari NN, Naghdi S, Fakhari Z, Komesh S, & Dommerholt. J:. Dry needling for hamstring flexibility: a single-blind randomized controlled trial. J Sport Rehabil. Advance online publication.
- Bandy W, Nelson R, Beamer L. 2017. Comparison of dry needling vs. sham on the performance of vertical jump. Int J Sports Phys Ther. 12:747-751.
- Brewster, B. D., Valier, A. R. S., & Falsone, S. (2021). A Systematic Dry Needling Treatment Supports Recovery Post-Training for Division I Ice Hockey Athletes: An Exploration Case Series. J Athl Train. https://doi.org/10.4085/1062-6050-0096.21
- Ceballos-Laita, L., Medrano-de-la-Fuente, R., Estébanez-De-Miguel, E., Moreno-Cerviño, J., Mingo-Gómez, M. T., Hernando-Garijo, I., & Jiménez-Del-Barrio, S. (2021). Effects of Dry Needling in Teres Major Muscle in Elite Handball Athletes. A Randomised Controlled Trial. J Clin Med, 10(18). https://doi.org/10.3390/jcm10184260
- Chiu, Y. C., Manousakas, I., Kuo, S. M., Shiao, J. W., & Chen, C. L. (2020). Influence of quantified dry cupping on soft tissue compliance in athletes with myofascial pain syndrome. PLoS One, 15(11), e0242371
- Decoster LC, Cleland J, Altieri C. 2005. The effects of hamstring stretching on range of motion: A systematic review. J Orthop Sports Phys Ther. 35:377-387.
- Ekhtiari S, Yusuf I, AlMakadma Y, MacDonald A, Leroux T, Khan M. 2020. Opioid Use in Athletes: A Systematic Review. Sports Health. 12:534-539.
- Ershad N, Ansari NN, Naghdi S, Otadi Kh, Gorji E, Dommerholt J. The effects of dry needling as a novel recovery strategy on quadriceps muscle fatigue: a pilot study. J Iran Med Counc. 2019;2(6):215-221.
- Ge HY, Nie H, Madeleine P, Danneskiold-Samsøe B, Graven-Nielsen T, Arendt-Nielsen L. 2009. Contribution of the local and referred pain from active myofascial trigger points in fibromyalgia syndrome. Pain 147:233-240.
- Ge HY, Arendt-Neilsen L, Madeleine P. 2012. Accelerated muscle fatigability of latent myofascial trigger points in humans. Pain Med. 13:957-964.
- Gerwin RD. 2008. The taut band and other mysteries of the trigger point: An examination of the mechanisms relevant to the development and maintenance of the trigger point. J Musculoskeletal Pain. 16, 115-121.
- Haser C, Stöggl T, Kriner M, Jörg M, Wolfahrt B, Scherr J, Halle M, Pfab F. 2017. Effect of Dry Needling on Thigh Muscle Strength and Hip Flexion in Elite Soccer Players. Med Sci Sports Exerc. 49(2):378-383.
- Hidalgo-Lozano, A., Fernández-de-las-Peñas, C., Alonso-Blanco, C., Ge, H.-Y., Arendt-Nielsen, L., & Arroyo-Morales, M. (2010). Muscle trigger points and pressure pain hyperalgesia in the shoulder muscles in patients with unilateral shoulder impingement: a blinded, controlled study. Experimental Brain Research, 202(4), 915-925. https://doi.org/10.1007/s00221-010-2196-4
- Hidalgo-Lozano, A., Fernandez-de-Las-Penas, C., Calderon-Soto, C., Domingo-Camara, A., Madeleine, P., & Arroyo-Morales, M. (2013). Elite swimmers with and without unilateral shoulder pain: mechanical hyperalgesia and active/latent muscle trigger points in neck-shoulder muscles. Scandinavian Journal of Medicine and Science in Sports, 23(1), 66-73. https://doi.org/10.1111/j.1600-0838.2011.01331.x
- Hui KK, Liu J, Makris N, Gollub RL, Chen AJ, Moore CI, Kennedy DN Rosen BR, Kwong KK. 2000. Acupuncture modulates the limbic system and subcortical gray structures of the human brain: evidence from fMRI studies in normal subjects. Hum Brain Mapp. 9:13-25.
- James SL, Ali K, Pocock C, Robertson C, Walkter J, Bell J, Connell D. 2007. Ultrasound-guided dry needling and autologous blood injection for patellar tendinosis. Br J Sports Med. 41:518-521.
- Jungmalm, J., Nielsen, R., Desai, P., Karlsson, J., Hein, T., & Grau, S. (2020). Associations between biomechanical and clinical/anthropometrical factors and running-related injuries among recreational runners: a 52-week prospective cohort study. Inj Epidemiol, 7(1), 10. https://doi.org/10.1186/s40621-020-00237-2
- Kamali, F., Sinaei, E., & Morovati, M. (2019). Comparison of Upper Trapezius and Infraspinatus Myofascial Trigger Point Therapy by Dry Needling in Overhead Athletes With Unilateral Shoulder Impingement Syndrome. J Sport Rehabil, 28(3), 243-249. https://doi.org/10.1123/jsr.2017-0207
- Kubo K, Yajima H, Takayama M, Ikebukuro T, Mizoguchi H, Takakura N. 2010. Effects of acupuncture and heating on blood volume and oxygen saturation of human Achilles tendon in vivo. Euro J Appl Physiol. 109:545-550.
- Langevin HM, Bouffard NA, Badger GJ, Churchill DL, Howe AK. 2006. Subcutaneous tissue fibroblast cytoskeletal remodeling induced by acupuncture: evidence for a mechanotransduction-based mechanism. J Cell Physiol. 207(3): 767-774.
- Langevin HM, Bouffard NA, Badger GJ, Churchill DL, Badger GH. 2007. Connective tissue fibroblast response to acupuncture: dose-dependent effect of bidirectional needle rotation. J Altern Complement Med. 13:355-360.
- Larsson R, Oberg PA, Larsson SE. 1999. Changes of trapezius muscle blood flow and electromyography in chronic neck pain due to trapezius myalgia. Pain. 79(1):45-50.
- Lavelle W, Smith HS. 2007. Myofascial trigger points. Anesthesiol Clin. 25:841-851.
- Llamas-Ramos R, Pecos-Martín D, Gallego-Izquierdo T, Llamas-Ramos I, Plaza-Manzano G, Ortega-Santiago R, Cleland J, Fernández-de-Las-Peñas C. 2014. Comparison of the short-term outcomes between trigger point dry needling and trigger point manual therapy for the management of chronic mechanical neck pain: a randomized clinical trial. J Orthop Sports Phys Ther. 44:852-861.
- Musa, R. M., Hassan, I., Abdullah, M. R., Latiff Azmi, M. N., Abdul Majeed, A. P. P., & Abu Osman, N. A. (2022). A longitudinal analysis of injury characteristics among elite and amateur tennis players at different tournaments from electronic newspaper reports. Front Public Health, 10, 835119. https://doi.org/10.3389/fpubh.2022.835119
- Myer, G. D., Jayanthi, N., Difiori, J. P., Faigenbaum, A. D., Kiefer, A. W., Logerstedt, D., & Micheli, L. J. (2015). Sport Specialization, Part I: Does Early Sports Specialization Increase Negative Outcomes and Reduce the Opportunity for Success in Young Athletes? Sports Health, 7(5), 437-442. doi:10.1177/1941738115598747
- Noblet AJ, Gifford SM. 2007. The sources of stress experienced by professional Australian footballers. J Appl Sport Psychology. 10:1-13.
- Ortega-Santiago, R., Gonzalez-Aguado, A. J., Fernandez-de-Las-Penas, C., Cleland, J. A., de-la-Llave-Rincon, A. I., Kobylarz, M. D., & Plaza-Manzano, G. (2019). Pressure pain hypersensitivity and referred pain from muscle trigger points in elite male wheelchair basketball players. Braz J Phys Ther. https://doi.org/10.1016/j.bjpt.2019.05.008
- Osborne NJ, Gatt IT. 2010. Management of shoulder injuries using dry needling in elite volleyball players. Acupunct Med. 28:42-45.
- Paantjens, M. A. (2013). Dry needling en adductorenmanipulatie voor de behandeling van een voetballer met adductorgerelateerde liespijn. Ned Mil Genees Tijdschr, 66–61–68, 64-70.
- Passigli S, Plebani G, Poser A. 2016. Acute effects of dry needling on posterior shoulder tightness. A case report. Int J Sports Phys Ther. 11:254-263.
- Rha DW, Park GY, Kim YK, Kim MT, Lee SC. 2013. Comparison of the therapeutic effects of ultrasound-guided platelet-rich plasma injection and dry needling in rotator cuff disease: a randomized controlled trial. Clin Rehabil. 27:113-122.
- Ruf, L., Altmann, S., Graf, F., Romeike, C., Wirths, C., Wohak, O., & Härtel, S. (2022). Injury incidence, severity, and burden in elite youth soccer players – A 3-year prospective study. Journal of Science and Medicine in Sport, 25(9), 737-742. https://doi.org/10.1016/j.jsams.2022.06.003
- Salom-Moreno J, Ayuso-Casado B, Tamaral-Costa B, Sánchez-Miliá Z, Fernández-de-Las-Peñas C, Alburquerque-Sendín F. 2015. Trigger point dry needling and proprioception exercises for the management of chronic ankle instability: A randomized clinical trial. Evid Based Complement Alternat Med. 790209.
- Shah JP, Danoff JV, Desai MJ, Parikh S, Nakamura LY, Phillips TM, Gerber LH. 2008. Biochemicals associated with pain and inflammation are elevated in sites near to and remote from active myofascial trigger points. Arch Phys Med Rehabil. 89(1):16-23.
- Stults-Kolehmainen M, Bartholomew JB. 2012. Psychological stress impairs short-term muscular recovery from resistance exercise. Med Sci Sports Exerc. 11:2220-2227.
- Thompson, R., Prosell, M., & Timpka, T. (2021). Elite athletes’ experiences of musculoskeletal pain management using neuroanatomical dry needling: A qualitative study in Swedish track and field. Journal of Science and Medicine in Sport, 24(1), 46-51. https://doi.org/10.1016/j.jsams.2020.07.004
- Wu MT, Sheen JM, Chuang KH, Yang P, Chin SL, Tsai CY, Chen CJ, Liao JR, Lai PH, Chu KA, Pan HB, Yang CF. 2002. Neuronal specificity of acupuncture response: A fMRI study with electroacupuncture. Neuroimage. 16:1028-1037.
- Yeste-Fabregat, M., Baraja-Vegas, L., Vicente-Mampel, J., Pérez-Bermejo, M., Bautista González, I. J., & Barrios, C. (2021). Acute Effects of Tecar Therapy on Skin Temperature, Ankle Mobility and Hyperalgesia in Myofascial Pain Syndrome in Professional Basketball Players: A Pilot Study. Int J Environ Res Public Health, 18(16). https://doi.org/10.3390/ijerph18168756