Introduction to Neck Pain and Prevalence
Up to 70% of the population will have neck pain at some time in their life (Côté et al. 2004), and neck pain is the fourth leading cause of disability in the United States after back pain, depression, and other musculoskeletal disorders (Murray et al. 2013). In other words, it is more than just a simple pain in the neck. A common complaint of those with neck pain is soreness in neck muscles that can affect their ability to turn the head and complete even the simplest daily tasks. While acute non-specific neck pain typically resolves without intervention, several factors have been associated with the persistence of neck pain, including being female, of older age, showing radicular signs, having a higher baseline pain intensity, a history of smoking, obesity, psychosocial factors, and having pain in multiple sites (Vos et al. 2008).
and neck pain is the fourth leading cause of disability in the United States after back pain, depression, and other musculoskeletal disorders (Murray et al. 2013). In other words, it is more than just a simple pain in the neck. A common complaint of those with neck pain is soreness in neck muscles that can affect their ability to turn the head and complete even the simplest daily tasks. While acute non-specific neck pain typically resolves without intervention, several factors have been associated with the persistence of neck pain, including being female, of older age, showing radicular signs, having a higher baseline pain intensity, a history of smoking, obesity, psychosocial factors, and having pain in multiple sites (Vos et al. 2008).
Muscular Involvement in Neck Pain
Neck muscles can be a primary source of neck pain either through direct injury (e.g., whiplash associated disorders), repetitive overuse injuries (e.g., postural strain), or direct injury (e.g., sports injuries). Alternatively, neck muscles can become a secondary source of neck pain when pain is present in other body areas. Neck pain has been shown to occur along with other painful conditions such as temporomandibular disorders, headaches, low-back pain, and joint pain (Vos et al. 2008). What is it, though, that makes neck muscles a source of pain?
Muscle Strain
Alterations in resting head posture can be a source of strain placed on the neck muscles that causes them to become overused or overloaded leading to pain. Prolonged sitting in a forward head and neck flexed posture has been shown to increase the biomechanical stress at the seventh cervical and first thoracic vertebrae during a five-minute reading task (Hamaoui et al. 2016). Researchers have tried to quantify the amount of strain placed on neck muscles by examining the ratio of the gravitational moment acting on the head that would tend to pull it forward to the muscle moment needed to counteract that forward force. They found that the moment needed to counteract the forward force can change up to 3–5 fold depending on the  task and body position (Hamaoui et al. 2016). Prolonged forward head and neck flexed positions and postures can increase biomechanical stress on the soft tissues and muscles of the head and neck (Vasavada et al. 2015). Some occupations that require more sitting or forward head bending, such as office workers and dentists are associated with a higher prevalence of neck pain (Hayes et al. 2009; Jun et al. 2017), and there is a rising incidence of neck pain with the advent of mobile device use. Even ten minutes of device use in sitting has been associated with increased neck discomfort in individuals with and without neck pain (Xie et al. 2016).
task and body position (Hamaoui et al. 2016). Prolonged forward head and neck flexed positions and postures can increase biomechanical stress on the soft tissues and muscles of the head and neck (Vasavada et al. 2015). Some occupations that require more sitting or forward head bending, such as office workers and dentists are associated with a higher prevalence of neck pain (Hayes et al. 2009; Jun et al. 2017), and there is a rising incidence of neck pain with the advent of mobile device use. Even ten minutes of device use in sitting has been associated with increased neck discomfort in individuals with and without neck pain (Xie et al. 2016).
Trigger Points
When a muscle is chronically overloaded or overused, such as through a prolonged forward head posture, trigger points can develop. A trigger point is a hyperirritable spot within a muscle contracture that can be spontaneously painful or when compressed or stretched. Trigger points can refer pain to other areas away from the muscle in somewhat predictable ways (Donnelly et al. 2019). While the exact mechanisms underlying trigger point formation and perpetuation are unknown, the integrated trigger point hypothesis proposes that an initiating event that stresses a muscle can lead to hypoxia within the muscle (Gerwin et al. 2004).
In the case of neck pain, the initiating event could be a chronic postural strain or a traumatic event, such as whiplash. Regardless of the initiating event, local chemical changes occur within the muscle, and pain receptors become activated. Then follows a cascade of biochemical changes that lead to reduced blood flow, an acidic pH, and eventual excessive acetylcholine levels that may explain the excessive contraction of local muscle fibers and the development of taut bands within the muscle. Over time, if not resolved, these changes can lead to sensitization of the peripheral and central nervous system and expansion of pain in the body beyond the original site of injury (Dommerholt 2011).
Trigger points associated with neck pain can occur in superficial and deep muscles of the neck. There is a growing body of evidence to support that changes occur both in the morphology of deeper neck muscles in individuals with the whiplash-associated disorder and in the ability to activate deep neck muscles in individuals with chronic neck pain.
Neck Pain Analysis and Findings
From a morphology perspective, magnetic resonance imaging studies of the deep neck muscles have shown that following neck injury, both deep extensor and deep flexor neck muscles can develop fatty infiltrates within the muscle tissue (Elliott et al. 2006; Elliott et al. 2010). For the deep extensor muscles, these changes have been shown to be greater in the suboccipital muscles (rectus capitis posterior minor/major) and the multifidi muscles, particularly at the C3 spinal level (Elliott et al. 2006), which can affect their ability to develop contractile force.
From an activation perspective, individuals with chronic neck pain can show a reduced ability to activate their deep neck flexor muscles, specifically the longus capitis and colli muscles, compared to healthy controls (Jull et al. 2004). This reduction in activation of the deeper neck muscles may lead to reduced neck stabilization, which could help to explain the persistence of neck pain in some individuals. A reduced ability to stabilize and support the cervical spine may promote further strain on the soft tissues and joints of the spine. Given that these changes in muscle composition and activation occur in the deeper neck muscles in individuals with chronic neck pain, this can present challenges to treatment.
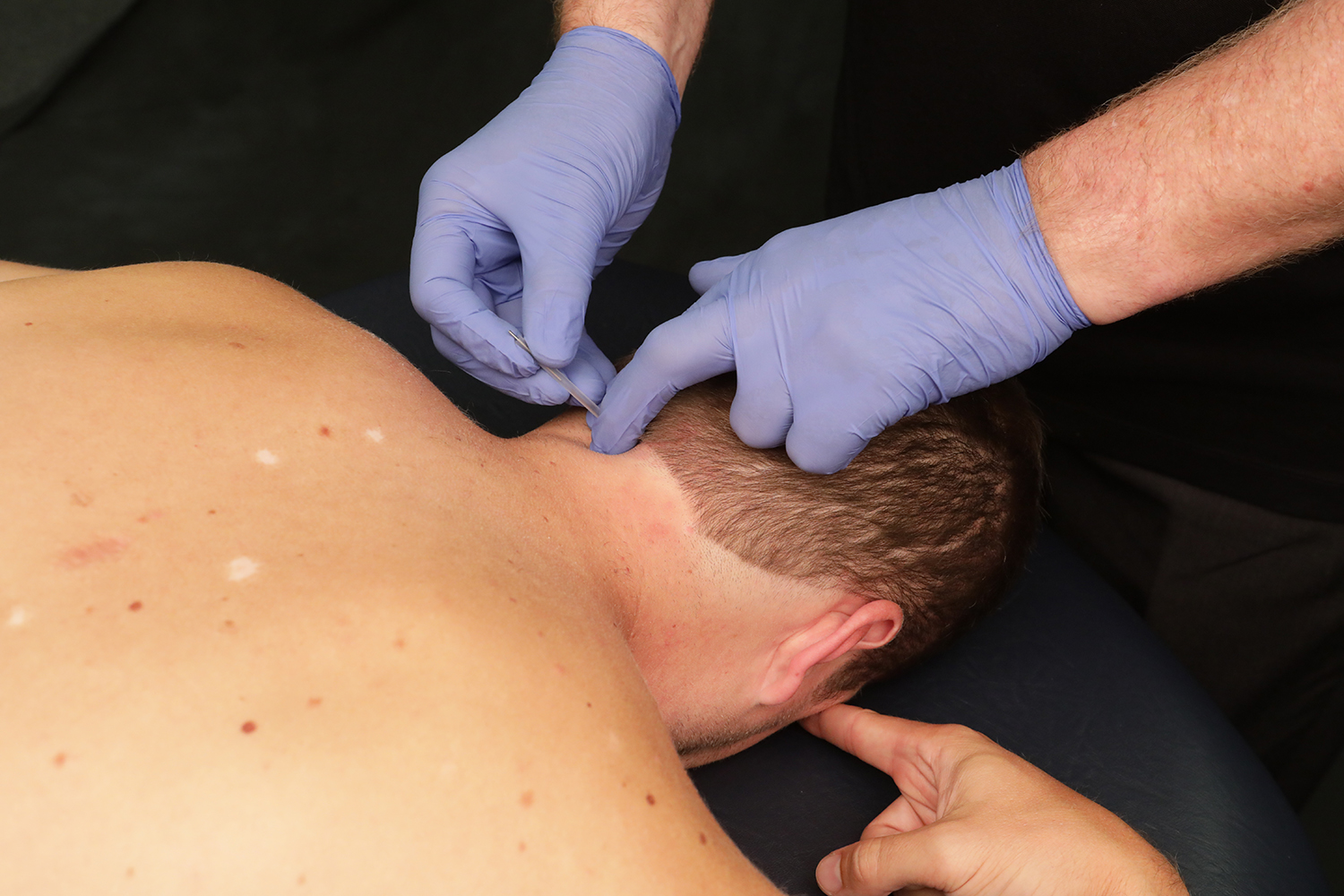
Dry Needling and Neck Pain
Evidence-supported approaches to treating neck pain include manual therapy, stretching, and strengthening (Blanpied et al. 2017). Additionally, dry needling has been recommended for use as part of a multimodal approach to treating chronic neck pain in individuals with mobility deficits (Blanpied et al. 2017). Dry needling is a skilled intervention using a thin filiform needle to penetrate the skin and stimulate a trigger point to produce a local twitch response. Dry needling of one large neck muscle, the trapezius, in people without neck pain has been shown to increase blood flow and oxygen saturation in the muscle (Cagnie et al. 2012).
strengthening (Blanpied et al. 2017). Additionally, dry needling has been recommended for use as part of a multimodal approach to treating chronic neck pain in individuals with mobility deficits (Blanpied et al. 2017). Dry needling is a skilled intervention using a thin filiform needle to penetrate the skin and stimulate a trigger point to produce a local twitch response. Dry needling of one large neck muscle, the trapezius, in people without neck pain has been shown to increase blood flow and oxygen saturation in the muscle (Cagnie et al. 2012).
In people with neck pain, there is a growing body of evidence to support positive effects of a combination of dry needling with other interventions for improving key impairments, specifically pain intensity, pain-related disability, pressure pain thresholds, and neck motion (Liu et al. 2015; Gallego-Sendarrubias et al. 2020; Navarro-Santana et al. 2020; Fernández-De-Las-Peñas et al. 2021). A combination of trigger point dry needling with pain neuroscience education has also been shown to be more effective at reducing pain intensity, disability, fear of movement, and pain anxiety than usual care in individuals with chronic neck pain (Valiente-Castrillo et al. 2021). Additionally, dry needling and passive stretching compared to stretching alone has been shown to significantly reduce pain intensity, pressure sensitivity, and perceived neck disability, as well as to improve neck active range of motion and muscle strength both in the short term and up to 6 months post-intervention (Cerezo-Téllez et al. 2016). However, understanding how dry needling most optimally fits into a comprehensive treatment program for neck dysfunction is ongoing.
A recent randomized controlled trial in individuals with neck pain compared dry needling to sham needling and found that dry needling provided no additional benefit compared to sham needling when added to a multimodal treatment program that already included manual therapy and exercise (Gattie et al. 2021). Despite some lack of clarity in how the researchers performed dry needling in that study if the results are valid, it suggests that adding dry needling to an already comprehensive program may produce no added benefit. However, when compared to other treatments such as manual trigger point treatment, evidence suggests that dry needling may offer additional beneficial outcomes. For example, while both manual trigger point treatment and trigger point dry needling in individuals with neck pain can lead to reduced pain and improved function and cervical motion, trigger point dry needling also can positively affect pressure sensitivity, while manual trigger point treatment does not (Llamas-Ramos et al. 2014).
The Benefits of Dry Needling
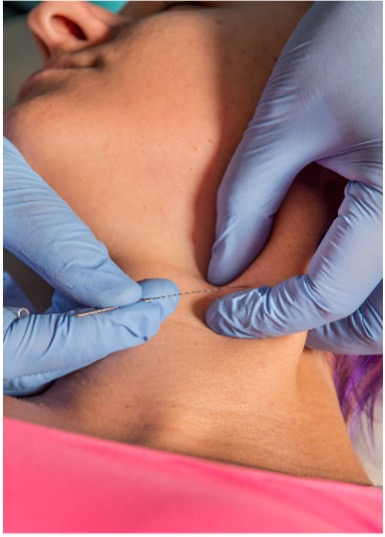 One of the benefits of dry needling in the cervical area is reaching deeper structures such as the deep neck flexor and extensor muscles. However, there is a paucity of evidence to show precisely how dry needling of the deeper neck muscles affects recovery, specifically muscle morphology and activation. In individuals with a whiplash-associated disorder, dry needling of the more superficial neck extensor muscles (trapezius, levator scapulae, splenius capitis, semispinalis, and spinalis capitis muscles) showed improved pain-related disability, pain catastrophizing, and cold hyperalgesia at 6 and 12 months follow-up compared to sham needling (Sterling et al. 2015).
One of the benefits of dry needling in the cervical area is reaching deeper structures such as the deep neck flexor and extensor muscles. However, there is a paucity of evidence to show precisely how dry needling of the deeper neck muscles affects recovery, specifically muscle morphology and activation. In individuals with a whiplash-associated disorder, dry needling of the more superficial neck extensor muscles (trapezius, levator scapulae, splenius capitis, semispinalis, and spinalis capitis muscles) showed improved pain-related disability, pain catastrophizing, and cold hyperalgesia at 6 and 12 months follow-up compared to sham needling (Sterling et al. 2015).
For individuals who are too irritable at the neck to tolerate palpation of muscle or needle insertion, there is evidence that dry needling of trigger points away from the neck can positively influence neck symptoms (Tsai et al. 2010). For example, in individuals with active trigger points in the upper trapezius muscle of the neck, dry needling of trigger points in the wrist extensor muscles has been shown to produce reduced pain sensitivity in the neck and improved range of neck motion (Tsai et al. 2010). When used appropriately as part of a comprehensive treatment program, dry needling can help individuals with neck pain to regain their pain-free function. However, one key to successful maintenance of pain-free function is likely to be the adoption of strategies that lessen the strain on the muscles of the head and neck.
Certified Cervical & Temporomandibular Therapist (CCTT) by the Physical Therapy Board of Craniofacial & Cervical Therapeutics
Certified Myofascial Trigger Point Therapist by Myopain Seminars
Dry Needling Course Series
The Dry Needling 1 course is an excellent starting point for learning the fundamentals of dry needling therapy. With a focus on the safe and effective application of dry needling techniques, you will gain a solid understanding of myofascial trigger points, needling techniques, precautions, and how to apply these techniques in clinical practice.
The Dry Needling 2 course is an intermediate-level course that provides in-depth knowledge and hands-on training for dry needling techniques of the extremities, including the upper and lower body. By completing this course, you will expand upon the skills you acquired in the DN-1 course and better understand the application of dry needling for managing musculoskeletal pain and dysfunction.
The Dry Needling 3 course is the final course in the series and the last step before becoming a Certified Myofascial Trigger Point Therapist – Dry Needling (CMTPT/DN). This course offers an in-depth study of advanced dry needling techniques for hand muscles, several lower extremity and foot muscles, the craniofacial and craniomandibular muscles, and more.
References
Blanpied, PR, Gross, AR, Elliott, JM, Devaney, LL, Clewley, D, Walton, DM, Sparks, C, Robertson, EK. Neck Pain: Revision 2017. J Orthop Sports Phys Ther 2017; 47(7): A1-a83.
Cagnie, B, Barbe, T, De Ridder, E, Van Oosterwijck, J, Cools, A, Danneels, L. The influence of dry needling of the trapezius muscle on muscle blood flow and oxygenation. J Manipulative Physiol Ther 2012; 35(9): 685-691.
Cerezo-Téllez, E, Torres-Lacomba, M, Fuentes-Gallardo, I, Perez-Muñoz, M, Mayoral-Del-Moral, O, Lluch-Girbés, E, Prieto-Valiente, L, Falla, D. Effectiveness of dry needling for chronic nonspecific neck pain: a randomized, single-blinded, clinical trial. Pain 2016; 157(9): 1905-1917.
Côté, P, Cassidy, DJ, Carroll, LJ, Kristman, V. The annual incidence and course of neck pain in the general population: a population-based cohort study. Pain 2004; 112(3): 267-273.
Dommerholt, J. Dry needling – peripheral and central considerations. J Man Manip Ther 2011; 19(4): 223-227.
Donnelly, JM, Fernandez-de-Las-Penas, C, Finnegan, M, Freeman, JL. Travell, Simons & Simons Myofascial Pain and Dysfunction. The Trigger Point Manual. Philadelphia, PA, Wolters Kluwer; 2019. pages.
Elliott, J, Jull, G, Noteboom, JT, Darnell, R, Galloway, G, Gibbon, WW. Fatty infiltration in the cervical extensor muscles in persistent whiplash-associated disorders: a magnetic resonance imaging analysis. Spine (Phila Pa 1976) 2006; 31(22): E847-855.
Elliott, JM, O’Leary, S, Sterling, M, Hendrikz, J, Pedler, A, Jull, G. Magnetic resonance imaging findings of fatty infiltrate in the cervical flexors in chronic whiplash. Spine (Phila Pa 1976) 2010; 35(9): 948-954.
Fernández-De-Las-Peñas, C, Plaza-Manzano, G, Sanchez-Infante, J, Gómez-Chiguano, GF, Cleland, JA, Arias-Buría, JL, López-de-Uralde-Villanueva, I, Navarro-Santana, MJ. Is Dry Needling Effective When Combined with Other Therapies for Myofascial Trigger Points Associated with Neck Pain Symptoms? A Systematic Review and Meta-Analysis. Pain Res Manag 2021; 2021: 8836427.
Gallego-Sendarrubias, GM, Rodríguez-Sanz, D, Calvo-Lobo, C, Martín, JL. Efficacy of dry needling as an adjunct to manual therapy for patients with chronic mechanical neck pain: a randomised clinical trial. Acupunct Med 2020; 38(4): 244-254.
Gattie, E, Cleland, JA, Pandya, J, Snodgrass, S. Dry Needling Adds No Benefit to the Treatment of Neck Pain: A Sham-Controlled Randomized Clinical Trial With 1-Year Follow-up. J Orthop Sports Phys Ther 2021; 51(1): 37-45.
Gerwin, RD, Dommerholt, J, Shah, JP. An expansion of Simons’ integrated hypothesis of trigger point formation. Curr Pain Headache Rep 2004; 8(6): 468-475.
Hamaoui, A, Hassaine, M, Watier, B, Zanone, PG. Effect of seat and table top slope on the biomechanical stress sustained by the musculo-skeletal system. Gait Posture 2016; 43: 48-53.
Hayes, M, Cockrell, D, Smith, DR. A systematic review of musculoskeletal disorders among dental professionals. Int J Dent Hyg 2009; 7(3): 159-165.
Jull, G, Kristjansson, E, Dall’Alba, P. Impairment in the cervical flexors: a comparison of whiplash and insidious onset neck pain patients. Man Ther 2004; 9(2): 89-94.
Jun, D, Zoe, M, Johnston, V, O’Leary, S. Physical risk factors for developing non-specific neck pain in office workers: a systematic review and meta-analysis. Int Arch Occup Environ Health 2017; 90(5): 373-410.
Liu, L, Huang, QM, Liu, QG, Ye, G, Bo, CZ, Chen, MJ, Li, P. Effectiveness of dry needling for myofascial trigger points associated with neck and shoulder pain: a systematic review and meta-analysis. Arch Phys Med Rehabil 2015; 96(5): 944-955.
Llamas-Ramos, R, Pecos-Martín, D, Gallego-Izquierdo, T, Llamas-Ramos, I, Plaza-Manzano, G, Ortega-Santiago, R, Cleland, J, Fernández-de-Las-Peñas, C. Comparison of the short-term outcomes between trigger point dry needling and trigger point manual therapy for the management of chronic mechanical neck pain: a randomized clinical trial. J Orthop Sports Phys Ther 2014; 44(11): 852-861.
Murray, CJ, Atkinson, C, Bhalla, K, Birbeck, G, Burstein, R, Chou, D, Dellavalle, R, Danaei, G, Ezzati, M, Fahimi, A, Flaxman, D, Foreman, Gabriel, S, Gakidou, E, Kassebaum, N, Khatibzadeh, S, Lim, S, Lipshultz, SE, London, S, Lopez, MacIntyre, MF, Mokdad, AH, Moran, A, Moran, AE, Mozaffarian, D, Murphy, T, Naghavi, M, Pope, C, Roberts, T, Salomon, J, Schwebel, DC, Shahraz, S, Sleet, DA, Murray, Abraham, J, Ali, MK, Atkinson, C, Bartels, DH, Bhalla, K, Birbeck, G, Burstein, R, Chen, H, Criqui, MH, Dahodwala, Jarlais, Ding, EL, Dorsey, ER, Ebel, BE, Ezzati, M, Fahami, Flaxman, S, Flaxman, AD, Gonzalez-Medina, D, Grant, B, Hagan, H, Hoffman, H, Kassebaum, N, Khatibzadeh, S, Leasher, JL, Lin, J, Lipshultz, SE, Lozano, R, Lu, Y, Mallinger, L, McDermott, MM, Micha, R, Miller, TR, Mokdad, AA, Mokdad, AH, Mozaffarian, D, Naghavi, M, Narayan, KM, Omer, SB, Pelizzari, PM, Phillips, D, Ranganathan, D, Rivara, FP, Roberts, T, Sampson, U, Sanman, E, Sapkota, A, Schwebel, DC, Sharaz, S, Shivakoti, R, Singh, GM, Singh, D, Tavakkoli, M, Towbin, JA, Wilkinson, JD, Zabetian, A, Murray, Abraham, J, Ali, MK, Alvardo, M, Atkinson, C, Baddour, LM, Benjamin, EJ, Bhalla, K, Birbeck, G, Bolliger, I, Burstein, R, Carnahan, E, Chou, D, Chugh, SS, Cohen, A, Colson, KE, Cooper, LT, Couser, W, Criqui, MH, Dabhadkar, KC, Dellavalle, RP, Jarlais, Dicker, D, Dorsey, ER, Duber, H, Ebel, BE, Engell, RE, Ezzati, M, Felson, DT, Finucane, MM, Flaxman, S, Flaxman, AD, Fleming, T, Foreman, Forouzanfar, MH, Freedman, G, Freeman, MK, Gakidou, E, Gillum, RF, Gonzalez-Medina, D, Gosselin, R, Gutierrez, HR, Hagan, H, Havmoeller, R, Hoffman, H, Jacobsen, KH, James, SL, Jasrasaria, R, Jayarman, S, Johns, N, Kassebaum, N, Khatibzadeh, S, Lan, Q, Leasher, JL, Lim, S, Lipshultz, SE, London, S, Lopez, Lozano, R, Lu, Y, Mallinger, L, Meltzer, M, Mensah, GA, Michaud, C, Miller, TR, Mock, C, Moffitt, TE, Mokdad, AA, Mokdad, AH, Moran, A, Naghavi, M, Narayan, KM, Nelson, RG, Olives, C, Omer, SB, Ortblad, K, Ostro, B, Pelizzari, PM, Phillips, D, Raju, M, Razavi, H, Ritz, B, Roberts, T, Sacco, RL, Salomon, J, Sampson, U, Schwebel, DC, Shahraz, S, Shibuya, K, Silberberg, D, Singh, JA, Steenland, K, Taylor, JA, Thurston, GD, Vavilala, MS, Vos, T, Wagner, GR, Weinstock, MA, Weisskopf, MG, Wulf, S, Murray. The state of US health, 1990-2010: burden of diseases, injuries, and risk factors. Jama 2013; 310(6): 591-608.
Navarro-Santana, MJ, Sanchez-Infante, J, Fernández-de-Las-Peñas, C, Cleland, JA, Martín-Casas, P, Plaza-Manzano, G. Effectiveness of Dry Needling for Myofascial Trigger Points Associated with Neck Pain Symptoms: An Updated Systematic Review and Meta-Analysis. J Clin Med 2020; 9(10).
Sterling, M, Vicenzino, B, Souvlis, T, Connelly, LB. Dry-needling and exercise for chronic whiplash-associated disorders: a randomized single-blind placebo-controlled trial. Pain 2015; 156(4): 635-643.
Tsai, CT, Hsieh, LF, Kuan, TS, Kao, MJ, Chou, LW, Hong, CZ. Remote effects of dry needling on the irritability of the myofascial trigger point in the upper trapezius muscle. Am J Phys Med Rehabil 2010; 89(2): 133-140.
Valiente-Castrillo, P, Martín-Pintado-Zugasti, A, Calvo-Lobo, C, Beltran-Alacreu, H, Fernández-Carnero, J. Effects of pain neuroscience education and dry needling for the management of patients with chronic myofascial neck pain: a randomized clinical trial. Acupunct Med 2021; 39(2): 91-105.
Vasavada, AN, Nevins, DD, Monda, SM, Hughes, E, Lin, DC. Gravitational demand on the neck musculature during tablet computer use. Ergonomics 2015; 58(6): 990-1004.
Vos, CJ, Verhagen, AP, Passchier, J, Koes, BW. Clinical course and prognostic factors in acute neck pain: an inception cohort study in general practice. Pain Med 2008; 9(5): 572-580.
Xie, Y, Szeto, GP, Dai, J, Madeleine, P. A comparison of muscle activity in using touchscreen smartphone among young people with and without chronic neck-shoulder pain. Ergonomics 2016; 59(1): 61-72.