Is surgery your only option?
Physical therapists commonly see patients with musculoskeletal pain and dysfunction. Many patients consulted previously with medical specialists, such as orthopedic surgeons or neurosurgeons, and often, they were told that they would need surgery to reduce pain and restore function. While in some cases, surgery may indeed be the best option, there are several scenarios where surgery may not necessarily be the optimal treatment of choice. Physical therapy may offer a more conservative and less expensive alternative.
Comparison of Physical Therapy and Surgery in Recent Studies
Degenerative Meniscal Tears with Arthroscopic Partial Meniscectomy
Let’s take a look at a recent study of 321 patients aged 45 to 72 years, that compared the effect of physical therapy on degenerative meniscal tears with arthroscopic partial meniscectomy [1]. The patients were randomly assigned to a surgery group or a physical therapy group and they were followed for five years. Patients in the physical therapy group followed a treatment protocol consisting of a physical therapist-led incremental exercise program over a period of 8 weeks, consisting of 16 sessions of 30 minutes each. Patients in the surgical group received written postoperative instructions, including a home exercise program. They were only referred for physical therapy if they showed a delayed recovery at an 8-week follow-up visit. In the end, 139 patients in each group completed the study. After 5 years, knee function in exercise-based physical therapy was not inferior to the outcomes of arthroscopic partial meniscectomy. Interestingly, the researchers found a small and comparable rate of progression of radiographic and symptomatic OA between both treatments. They concluded that exercise-based physical therapy should be the preferred treatment over surgery for degenerative meniscal tears [1].
A systematic review of 17 studies (2037 patients) also concluded that there are only limited benefits to performing arthroscopic partial meniscectomy in adults diagnosed with degenerative and nonobstructive meniscal symptoms [2]. Physical therapy produced comparable results to surgery and should be recommended before considering surgical options [2].
Both studies question why patients with degenerative meniscal tears would be considered for surgery before exploring other options, especially, because a review of the current literature, indications, and outcomes of partial meniscectomy failed to demonstrate substantial benefits of surgery over nonoperative treatments or even placebo surgery [3]. A Finnish study compared arthroscopic partial meniscectomy with placebo surgery and after 5 years, they found only a slightly increased risk of developing radiographic knee osteoarthritis and no concomitant benefit in patient-relevant outcomes [4]. Of interest in this context is the book “Surgery, the Ultimate Placebo” by Ian Harris [5], who concluded that many of the commonly performed surgeries were no better than placebo! Click here for an interesting interview by Dr. Wael Mahmoud from Melbourne, Australia (who happens to be the only Myopain Seminars CMTPT/DN in the entire Australian continent).
Lumbar Spinal Stenosis
Another study of 224 patients diagnosed with lumbar spinal stenosis compared supervised physical therapy to surgery [6]. Although at first glance, the surgical group appeared to do better on claudication symptoms, pain, and functioning, after adjusting the two groups based on the severity of symptoms, there were no significant differences in baseline characteristics and all clinical outcomes at 1 year. The authors concluded that in mild to moderate cases of lumbar spinal stenosis, supervised physical therapy is preferred over surgery as a first-choice treatment to prevent complications and minimize health care costs [6].
A systematic review and meta-analysis comparing exercise vs. surgery in improving the quality of life, pain, and disability of patients with large to massive rotator cuff tears concluded that exercise was as effective as surgery [7]! The researcher remarked, however, that there is a paucity of high-quality research on the role of exercise and which exercises may be most beneficial [7].
Femoroacetabular Impingement Syndrome
Yet, another study of patients suffering from femoroacetabular impingement syndrome concluded that arthroscopic hip surgery resulted in improving quality of life and activity of daily living, but there was no difference in functional sports performance compared to conservative therapy [8]. The outcomes of exercise therapy were maintained at a follow-up of 4.6 years in 26 patients with femoroacetabular impingement syndrome with did not undergo hip surgery [9].
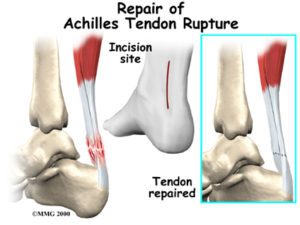 Acute Achilles’ Tendon Rupture
Acute Achilles’ Tendon Rupture
Perhaps even more surprising, a study of 526 patients with an acute Achilles’ tendon rupture established that open repair of minimally invasive surgery did not lead to better outcomes than non-operative treatments at 12 months [10].
Is Surgery The Best Choice?
In summary, surgery clearly is not necessarily the best choice for a variety of musculoskeletal injuries and conditions. To provide the quality of care for patients who received surgical recommendations, physical therapists must be able to provide a solid differential diagnostic and decision-making process and be able to communicate their findings and treatment plan. A collaborative or patient-centered approach may improve patient outcomes [11].
References
1. Noorduyn, J.C.A., et al., Effect of Physical Therapy vs Arthroscopic Partial Meniscectomy in People With Degenerative Meniscal Tears: Five-Year Follow-up of the ESCAPE Randomized Clinical Trial. JAMA Netw Open, 2022. 5(7): p. e2220394.
2. Migliorini, F., et al., No evidence in support of arthroscopic partial meniscectomy in adults with degenerative and nonobstructive meniscal symptoms: a level I evidence-based systematic review. Knee Surg Sports Traumatol Arthrosc, 2022.
3. Avila, A., et al., Current Controversies in Arthroscopic Partial Meniscectomy. Curr Rev Musculoskelet Med, 2022.
4. Sihvonen, R., et al., Arthroscopic partial meniscectomy for a degenerative meniscus tear: a 5 year follow-up of the placebo-surgery controlled FIDELITY (Finnish Degenerative Meniscus Lesion Study) trial. British Journal of Sports Medicine, 2020. 54(22): p. 1332.
5. Harris, I., Surgery, the ultimate placebo. 2016, Sydney, NSW: NewSouth Publishing.
6. Minetama, M., et al., Supervised physical therapy versus surgery for patients with lumbar spinal stenosis: a propensity score-matched analysis. BMC Musculoskelet Disord, 2022. 23(1): p. 658.
7. Fahy, K., et al., Exercise as effective as surgery in improving quality of life, disability, and pain for large to massive rotator cuff tears: A systematic review & meta-analysis. Musculoskelet Sci Pract, 2022. 61: p. 102597.
8. Mok, T.N., et al., Arthroscopic Hip Surgery versus Conservative Therapy on Femoroacetabular Impingement Syndrome: A Meta-Analysis of RCTs. Orthop Surg, 2021. 13(6): p. 1755-1764.
9. Monn, S., et al., Mid-term outcomes of exercise therapy for the non-surgical management of femoroacetabular impingement syndrome: are short-term effects persisting? Phys Ther Sport, 2022. 55: p. 168-175.
10. Myhrvold, S.B., et al., Nonoperative or Surgical Treatment of Acute Achilles’ Tendon Rupture. N Engl J Med, 2022. 386(15): p. 1409-1420.
11. Dwamena, F., et al., Interventions for providers to promote a patient-centred approach in clinical consultations. Cochrane Database Syst Rev, 2012. 12: p. CD003267.

